Pain & Injury Survival Tips
Dozens of ideas (and links) for evidence-based rehabilitation and self-treatment for common pain problems and injuries
Need some pain relief? Without a sales pitch? Here are the greatest hits from my brain, every self-treatment tip and tactic that I’ve ever recommended, everything that’s “worth a shot” because it’s relatively cheap, safe, and plausible — even if it’s not proven (on another page, I report on only the most evidence-based pain treatments — a much shorter list, alas). Plus there are practical warnings about the most important things to avoid. This compilation of tips comes from well over a decade of writing, research, experience, and truckloads of email with readers and experts.
When you have a painful and stubborn problem, the troubleshooting recipe is to learn as much as you can about the treatment options, and then start experimenting, working your way from the cheaper, easier, safer, more reasonable options to the more expensive, awkward, risky, kooky options. And skip the worst!
Browse the tips below to plan your approach to most healing and rehabilitation challenges, especially athletic injuries, overuse syndromes, muscular pain, joint pain, chronic pain, and repetitive strain syndromes. Almost every tip includes links to (way) more detailed articles and tutorials.
What makes a self-treatment worth trying?
Chronic pain matters. Its seriousness is often expressed in terms of the hair-raising economic costs of work absenteeism, but it may well be far worse than that — a recent Swedish study shows that it probably even shortens people’s lives.+Jansson C, Mittendorfer-Rutz E, Alexanderson K. Sickness absence because of musculoskeletal diagnoses and risk of all-cause and cause-specific mortality: A nationwide Swedish cohort study. Pain. 2012 May;153(5):998–1005. PubMed 22421427 ❐ And yet sadly, as you know, there are no magic bullets. Pain is hard to treat. In fact, there is not a single common painful problem that can be “fixed” reliably by any therapy. And many popular treatments actually fail miserably most of the time, or all of the time. I cannot tell you how often I have heard someone admit that they are still in pain, even though they are spending thousands of dollars on [insert popular therapy].
Despite the disappointing reality, there are many treatment approaches that are still “worth a shot” because they are relatively:
- plausible
- safe
- accessible (easy, cheap)
The less plausible, safe, easy, and cheap a treatment is, the more hard evidence we need that it actually works. That evidence is simply lacking for many expensive therapies. (No, science doesn’t have all the answers — but it’s a starting point.) I never recommend treatments that are actually dis-proven, seriously implausible, and/or risky — if you want that kind of advice, there are a lot of other places online that will be happy to give it to you.
However, I do recommend treatments that are reasonably harmless to you, your wallet, and your schedule … even if they aren’t exactly guaranteed to work. The focus here is on creative and sensible experimentation, on saving yourself without embracing quackery. Here’s how science writer Alex Hutchinson puts it, really capturing the spirit of this website:
I’m a big advocate of better science to really understand what causes injuries and how to treat them — but in practice, I also believe that sometimes it’s worth trying something, anything, just in case it successfully ‘reboots’ your injury.
Part 2
The Tips
Be aware: doctors may not know their aches & pains medicine
That’s not an anti-medical message: I am pro-doctor. I think griping about “mainstream medicine” is usually misguided (not that it’s perfect, duh). I’m pro-vaccine, I know that doctors are much better trained than naturopaths or chiropractors, and I think medical error rates are naïvely over-emphasized by quacks without a clue about the pressure cooker of impossible problems and no-win situations that doctors have to deal with.
But that doesn’t mean doctors are perfect or good at everything! And there’s one way that family doctors (or “general practitioners” in some countries) are particularly imperfect: musculoskeletal medicine, or aches and pains medicine.
Most doctors lack the skills and knowledge needed to care for common aches, pains, and injury problems, especially the chronic cases, which they tend to underestimate the complexity of. This has been shown by many studies, like Stockard et al., who found that 82% of medical graduates “failed to demonstrate basic competency in musculoskeletal medicine.” It’s just not their thing, and people with puzzling or stubborn pain should take their family doctor’s advice with a large grain of salt, and even lower their expectations of specialists (who tend to be too specialized). See The Medical Blind Spot for Aches, Pains & Injuries: Most physicians are unqualified to care for many common pain and injury problems, especially the more stubborn and tricky ones.
Be aware of sneaky causes of pain
For every relatively obvious cause of pain, there are several subtle and mysterious ones that are notoriously difficult to diagnose, and probably several more that are just totally unknown. Even in cases that seem straightforward — like a stubborn case of shin splints, say — there can be weird curveballs like sensitization that are the real key to the condition. It’s a good idea to for every patient with chronic pain to get familiar with some of these sneak sources of pain.
Information like this is real hypochondria fuel, so try not to get freaked out by the many possible nasty things. Remember that “when you hear hoofbeats in Texas, think horses not zebras” (a classic medical saying about applying Occam’s razor to diagnosis). Most chronic pain has nothing to do with any horrible disease. But, when you reach a certain level of desperation, risking hypochondria is probably the lesser of evils.
Most people who look at all the possibilities won’t find a match. But a few patients hit the jackpot and realize that their pain is caused by something completely fixable, like a drug side effect (a problem so common it is the subject of its own pain tip here). A few unlucky people will discover that their pain is the tip of a pathological iceberg. To review the range of possibilities, see 38 Surprising Causes of Pain: Trying to understand pain when there is no obvious explanation.
Reduce vulnerability to chronic pain
We crave specific explanations and solutions to our pain, but sometimes they simply don’t exist, or they are effectively impossible to diagnose. So what then? Cast a wide net!
Many important causes of pain are the general conditions in which it flourishes, the soils and fertilizers it likes. For instance, if the same minor structural problem with the spine can cause a lot of pain in some people, but only trivial or no pain at all in many others — which is definitely a thing! — then is it really a “spine” problem? The more basic issue is the underlying vulnerability to any kind of pain, which increases the risk of a minor glitch blooming into a chronic pain problem.
Some of the classic non-specific vulnerabilities — the ones you might be able to fix — are things like being out of shape, stress, insomnia, vitamin D deficiency, or a drug side effect. Many of the other tips on this page are already about reducing those vulnerabilities, while this “tip” is about giving you a good reason to pursue self-improvement projects that might otherwise seem excessively general, trite, or easier-said-than-done to the point of being useless. But the general answers probably actually do matter, and you should take them seriously, because this is actually how pain treatment works. Read more about non-specific vulnerality to pain.
The best evidence for treating persistent pain points towards improving general health, as opposed to fixing specific “issues in the tissues.”
Playing With Movement, by Todd Hargrove, p. 217
Trigger point massage: the best “secret” weapon, useful even when muscle pain is not the main problem
Muscle knots — myofascial “trigger points” — are a factor in most of the world’s aches and pains. Their biology is still mostly mysterious: conventional wisdom says they are tiny spasms, but they might also be more of a pure neurological problem. Regardless, they can cause strong pain that often spreads in confusing patterns, and they grow like weeds around other painful problems and injuries, making them quite interesting and tricky. Although they are well known to many specialists and researchers, most doctors and therapists know little about them, so misdiagnosis is epidemic.
Probably because of trigger points, simple self-massage is helpful for a surprising number of common pain problems. Even when trigger points are not the root cause of your problem, they may be aggravating it and producing some of the pain, so they are always worth considering even in cases that do not seem especially “knotty.” The main limitation, of course, is your reach! Self-massage is only useful if relevant trigger points can reasonably be reached by your own hands, with tools that you have improvised or purchased for the job, or with the help of a partner or spouse.
See my main trigger points tutorial. For an in-depth look at how muscles knots work and why they tend to make you feel weak, why they resist stretch, how they can be so stubborn, and why rubbing them probably works, see Micro Muscles and the Dance of the Sarcomeres. For some good basic information about self-treating muscle knots, see Basic Self-Massage Tips for Myofascial Trigger Points. Or check my “perfect spots” series, which describes several ideal spots in the human body for massage. Speaking of the spots …
Learn your perfect spots for pressure: a few key points go a long way
The big idea here — what makes this worthy of a tip — is not that there are particularly good spots for massage on the human body, but this: knowing a few of them is almost everything you need to know.
Have you ever heard of the 80-20 rule? The “law of the vital few”? In many situations, roughly 80% of the effects come from 20% of the causes. In massage, most of what you need comes from just a few of the most important and satisfying places to massage. Every decent massage therapist has an intuitive grasp of this, and it’s why we seem like we have “magic hands” — it’s actually not that hard to zoom in on the most important spots, because there are just not that many of them. Of course there are others, and the other 20% do matter. But understanding that a few key points are especially important can really make a difference in your approach … and it’s not nearly as hard to know where to press as you might think.
So start learning your spots!
The bath trick: give yourself a back rub with a ball in a bath
This is my favourite clever self-massage tip. It came from combining two other classic tactics for treating your own trigger points: the heat of a bath, with the pressure of a ball (see tennis ball massage). But the result is more than the sum of the parts, and it works better in some ways than any other method of self-massage method I’ve ever come up with. The idea is simply to run a hot bath, and trap a ball between your body and the bottom or back of the tub to rub your back muscles — your buoyancy allows for excellent control with moderate pressures.
And you need the right kind of ball for best results. See The Bath Trick for Trigger Point Release.
Prevention: important even after you’ve been hurt
A major part of healing is prevention: that is, the prevention of re-injury, and so “prevention” is actually relevant even after you’ve already gotten into trouble. Also, injury and pain problems tend to make people accident prone. When one ankle is sprained, it’s easier to trip and sprain the other one. This is called “collateral injury,” and is amazingly common.
Some collateral injuries are far worse than the original injury. Consider the case of a young woman who tripped and could not catch herself properly because of a shoulder injury, resulting in quite serious damage to her head and face. So, when you are hurting, it pays to make caution and prevention a higher priority than usual. Many of the strategies described below constitute prevention.
Microbreaking: mobilizations at work
Microbreaking is the strategy of taking small breaks from work and moving around to prevent the many deleterious effects of stillness. In particular, it’s an easy way to keep muscles from developing painful trigger points. It is a survival skill for every chair-bound office worker, student, computer user, or anyone at all whose work (or play) generally requires long hours of being sedentary. But here’s the nugget of the tip: just “taking a break” isn’t enough. Walking to the water cooler and back—while not a bad idea—does not constitute actual stimulation for back muscles that are screaming with stiffness. It is necessary to actually do something therapeutic with microbreaks, such as mobilizations, AKA joint mobility drills.
For a brief overview of microbreaking alone, see Microbreaking. For a complete survival guide for sedentary work, see The Trouble with Chairs.

“Piled Higher and Deeper” www.phdcomics.com by Jorge Cham
Endurance training: under-rated but vital therapeutic exercise
Endurance training is a weight-lifting workout that uses large numbers of “reps” and lighter loads: i.e. lifting a light barbell thirty times, instead of lifting a heavy barbell eight times. It is a sensible (low risk) default style for most women at the gym. Really, endurance training is just an intense kind of mobilization exercise (see above). Mobilizations are basically just very easy endurance training, and endurance training is just mobilizations with some light weights. It is a terrific way to get some exercise without risking aggravation of myofascial trigger points (muscle knots) — indeed, if done in moderation, without excessively exhausting yourself, it might be a therapy for trigger points. It is almost certainly a more effective self-treatment for muscle stiffness and pain than, say, stretching. I recommend endurance training exercises to people who aren’t sure what they should be doing at the gym while injured.
See Endurance Training for Pain & Rehab for more information.
Strength training: better, easier than you thought

Strength training is the high-load, low-rep load-bearing exercise at the gym that a few guys like to do — and most other people ignore. Please don’t! It can be a valuable component in rehabilitation. Done properly, challenging your muscles is more efficient and better for your general fitness that you probably think. It is a terrific way to get fit or stay fit without aggravating existing injuries or risking new ones. Universal gym equipment may be intimidating for beginners, but it offers important rehabilitation advantages: precise, safe control of which tissues you’re affecting. Many people might be much more willing to develop a gym habit if only they understood these benefits.
And yet conventional rehabilitative strength training certainly can be misguided and problematic: overdoing it, sloppy work with free weights, and training problem tissues directly instead of training around them are all risky. In particular, beware of the logic of trying to “strengthen the problem,” like exercising back muscles to treat low back pain: here be dragons! Strengthening may be quite ineffective as a treatment (see Don’t bother with hip strengthening).
For a full discussion of the pros, cons, hazards, and best practices, see Strength Training for Pain & Injury Rehab. To be persuaded that you can get surprisingly good benefits with not much time at the gym see, Strength Training Frequency: Less is more than enough: go to the gym less frequently but still gain strength fast enough for anyone but a bodybuilder. Or, if you just cannot stomach the gym, see the next section …
The scientific 7-minute workout
Getting as much exercise as possible is extremely important but also difficult and unappealing for people in chronic pain. Efficiency is critical! Fortunately, it’s also possible.
To get the most bang for your exercise buck, make a daily habit of the “Scientific 7-Minute Workout,” based on the principle that small, intense doses of exercise are surprisingly effective. It’s a well-rounded, efficient workout that requires only a chair and a few minutes of oomph: a dozen exercises, each performed for 30 seconds, with a brief break between each of them. The S7M workout can adapt nicely for compatibility with injury rehab. For instance, if you are recovering from a stubborn knee problem like patellofemoral syndrome, you can skip the exercises that stress the knee — exercising everything else as efficiently as possible.
The order of the exercises matters, and so does the oomph (it’s brief, not easy). Read about it and then try it: there are also dozens of apps, websites, and videos to guide you (though an egg-timer and a picture of the exercises works fine); the best I’ve found is www.7-min.com.
Stretching is most over-rated! But it may be useful for a few specific problems
Stretching is over-rated. Many studies have clearly shown that stretching just isn’t good for the things people assume it is (warmup and injury prevention, performance enhancement, treating soreness). And although it does increase flexibility, but most people don’t actually need to be more flexible. To be deprogrammed, see Quite a Stretch. It does feel nice, it can relieve acute cramps (obviously), and there might be some kinds of pain it can treat. But it’s applications are too few. If you have a stretching habit with unclear value, do yourself a favour and break it. I prefer to recommend yoga or Pilates (which are much more than just stretching), Mobilize! and Basic Self-Massage Tips for Myofascial Trigger Points.
Heating: the most basic comfort

For relaxation and moderate relief from aching muscle pain in a specific location, use heat in the form of heated gel packs, heating pads, Thermophores (a special heating pad), towels saturated in hot water, and so on. Full-body heating in hot tubs, showers, saunas, and steam rooms is also helpful, especially when emotional stress and/or knots in your muscles are the cause of your troubles, or a significant complicating factor. Generally speaking, do not heat recently damaged tissue such as ankle sprains or muscle tears. Both ice and heat may help neck and back pain, but you should usually choose heat: ice is more likely to aggravate cranky muscles, and usually can’t help because inflammation is either not present at all or simply too deep for the ice to reach. See (Almost) Never Use Ice on Low Back Pain! for details.
Please see Heat for Pain and Rehab for more information. See Hot Baths for Injury & Pain for tips on getting the most out of your bathtub or Jacuzzi. See Ice versus Heat for Pain and Injury for a bird’s eye view of heating and cooling ideas and information on PainScience.com.
Raw icing and power icing: for acute and chronic injuries

To reduce pain and swelling associated with any acute injury or tendinitis,† always use ice (and also elevate the injury above the heart if you can so that it can “drain”). Beware of assuming that neck or back pain are “injuries” that need icing — they usually aren’t (see (Almost) Never Use Ice on Low Back Pain!). Despite this, both ice and heat will usually help back and neck pain, and you should use whichever seems appealing to you.
“Tendinitis” versus “tendonitis”: Both spellings are acceptable these days, but the first is the more legitimate, while the second is just an old misspelling that has become acceptable only through popular use, which is a thing that happens in English. The word is based on the Latin “tendo” which has a genitive singular form of tendinis, and a combining form that is therefore tendin. (Source: Stedmans Electronic Medical Dictionary.)
“Tendinitis” vs “tendinopathy”: Both are acceptable labels for ticked off tendons. Tendinopathy (and tendinosis) are often used to avoid the implication of inflammation that is baked into the term tendinitis, because the condition involves no signs of gross, acute inflammation. However, recent research has shown that inflammation is actually there, it’s just not obvious. So tendinitis remains a fair label, and much more familiar to patients to boot.
Icing may help with tendinitis and other chronic overuse injuries, but not because of any anti-inflammatory effect: tendinitis isn’t an inflammatory condition, believe it or not. Nevertheless, ice may stimulate recovery by other means. For this kind of injury, try “power icing” — 20–50 applications of ice per day for 3–20 days at a time. (Quit early if it’s not helping.) As long as you allow sufficient opportunity for tissue to warm up between applications, this is a safe and easy way to try to stimulate tissues to heal.
Please see Icing for Injuries, Tendinitis, and Inflammation for detailed instructions, and some more handy tips, especially how to make a convenient icing tool out of a Styrofoam cup! See Ice versus Heat for Pain and Injury for a bird’s eye view of heating and cooling ideas and information on PainScience.com.
An important icing exception: please (almost) never ice low back pain!
Back pain is the number one common pain problem, and an ice pack is the first thing most people will reach for … but it’s usually a mistake. Back pain is rarely an injury — that is, the pain is rarely caused by inflammation which might be helped by ice. Even in cases where inflammation is present, it is usually deep in the back under a thick layer of insulating muscle, so the ice can’t “reach” it. However, back pain almost always involves muscular trigger points (muscle knots), which are more likely to be aggravated by ice and helped by heat! For this reason, the majority of people with back pain prefer heat, and a few have negative reactions to ice. For similar reasons, neck pain usually should also not be iced.
Although experiments have shown that both ice and heat are modestly helpful for low back and neck pain, there are good reasons to err on the side of heat. Ice should only be used on the back by patients who clearly prefer it (for whatever reason), or when there is definitely a fresh injury.
Please see (Almost) Never Use Ice on Low Back Pain! for more information. See Ice versus Heat for Pain and Injury for a bird’s eye view of heating and cooling ideas and information on PainScience.com.
Contrasting with heating and cooling: well worth a shot

Contrasting won’t work any miracles, but really hits the “reasonable, safe, easy, cheap” sweet spot. It is a worthwhile self-treatment for a wide variety of conditions that can benefit from an increase in stimulation and circulation: in other words, practically anything except fresh injuries. Gentle exercise and movement are the best ways of increasing circulation, but it isn’t always an option to exercise a body part that is already injured or teetering on the edge of an overuse injury. Contrasting is useful because it powerfully stimulates circulation without any significant risk of irritating tissue. (Please note again: it can’t be used on the freshest injuries, because acute inflammation is aggravated by heat.) Similarly, more intense full body contrasting — switching back and forth between hot tub and pool — is an exhausting “thermal workout,” ideal for wearing yourself out and burning some calories without straining anatomy. Contrasting involves alternating between soaking in hot water and soaking in cold. Always finish with cold. Use a double-sink, a pair of buckets, a detachable shower head ... or whatever arrangement you can dream up.
Please see Contrast Hydrotherapy for more information. See Ice versus Heat for Pain and Injury for a bird’s eye view of heating and cooling ideas and information on PainScience.com.
Epsom salt baths: the bath is nice, but the salt is useless
It’s a popular idea, but there is no good reason to believe that bathing in dissolved Epsom salts will have the slightest effect on muscle soreness or injury recovery time, or indeed any kind of therapeutic effect whatsoever. Although this folk wisdom may someday prove to have a sound rationale, clearly there is none that its advocates have thought of — or even tried to think of, it seems. It may be harmless, but it’s so implausible and stakes are so low that I think the verdict is a no-brainer: the smart money is on not bothering.
For a lot more detail — an absurd amount of detail, really — see Does Epsom Salt Work?
Extra water intake? Don’t worry about it

There is an epidemic of low-grade anxiety out there about whether or not we are drinking enough water, and I believe it’s all unnecessary. Alternative health care professionals constantly recommend this, and seem to assume that throwing back a couple extra litres of water a day is essential to virtually all rehabilitation and general health. But the question would not exist if it weren’t for the scientifically bankrupt work of Dr. Batmanghelidj, who almost single-handedly invented the “threat” of “chronic dehydration” as a social phenomenon. If the threat exists at all, it’s not serious: it’s easily cured with minimal extra hydration. There are more important things to worry about. Drink when you’re thirsty, or perhaps just slightly more, and ignore anyone who tries to get you too worried that it’s not enough.
For the whole sordid story, see Water Fever and the Fear of Chronic Dehydration.
Get more sleep! If you’ve got insomnia, start looking seriously for solutions
Sleep deprivation is an unsuspected and major aggravating factor in a great many cases of chronic pain or slow injury recovery. Indeed, you may be suffering some of the consequences of sleep deprivation even if you think that you are getting a “normal” amount of sleep with 6–7 hours per night. In his book Sleep Thieves, sleep scientist Stanley Coren of the University of British Columbia spells out just exactly how sleep deprived most people in our society probably are — and how much more significant the consequences may be than we realize. An increase in aches and pains, immune system suppression, and weight gain are three common side effects of relatively mild sleep deprivation. And if you are actually suffering from significant insomnia, it gets worse.
Of course, insomnia can be tough to beat, so see The Insomnia Guide for Chronic Pain Patients for some of the best sleep repair tips you can find (way beyond warm milk).
Sleep is like a cat: it only comes to you if you ignore it.
Gillian Flynn, Gone Girl
Tactical resting: the underestimated art of taking it easy
Surprisingly, rest is often underestimated or simply ignored as a factor in healing. However logistically awkward and emotionally frustrating proper rest can be, perpetual injury is worse. Particularly for overuse (repetitive strain) injuries, it is necessary to tackle rest like a major tactical challenge, and well-planned rest may be the only rehab strategy that offers any real hope of working. And yet almost no health care professionals or patients take such injuries “seriously” enough to inspire rest that is adequate and well-executed! In such cases, the injury is perpetually and tragically re-aggravated, often by a misguided fear that resting the injury will compromise general fitness. But fitness is harder to lose than people think, not such a big deal to rebuild, and in any case the greater evil is to remain injured. Failing to rest can easily lead to many years of chronic pain and reduced fitness. Yikes!
So how do you rest “tactically”? You particularly need relative rest, which involves remaining as active as you can — protecting your fitness — while protecting injured tissues as much as possible. Resting sounds simple, but it actually requires quite a lot of planning and savvy to do it properly, and psychological resistance can be fierce. For more of the why and how of resting, see The Art of Rest.
Nutrition for healing: possibly helpful for serious chronic pain
Obviously good nutrition is generally important to health, but this does not usually require vitamin and mineral supplementation. Despite the popular opinion to the contrary, modern food is actually quite nutritious, and most supplementation has turned out to be disappointingly futile. However, the point of this tip is much more specific: there are good reasons to believe that even relatively mild nutritional deficiencies may perpetuate or aggravate some mechanisms of chronic pain, like trigger points in muscle, thereby complicating virtually any painful condition. Therefore, consider a nutritional review when troubleshooting any mysterious or stubborn pain problem. Moderate supplementation might make a difference. While I would warn healthy people away from wasting money on supplements, I think issues of nutrition and supplements are worth considering for those suffering any kind of chronic pain.
More detailed information about nutrition on this website is available mainly in a chapter by of the advanced muscle pain tutorial. But Vitamin D stands out, and is covered in the next tip.
Be the kind of person who takes supplements — then skip the supplements.
Michael Pollan, Food Rules: An Eater’s Manual
Vitamin D: the most likely of all supplements to be useful for pain
For chronic pain patients specifically — not just anyone, but people with a genuine chronic pain to solve — vitamin D has real promise. There is still no proof yet that D deficiency can cause pain, or that D supplementation can treat pain. But there is enough indirect evidence connecting them to be of serious interest, and supplementation is safe and cheap. The maximum dosage commonly available over-the-counter in North America (5000 IU capsules of vitamin D3) is comfortably within the safe range.
Naturally, you should run this by your doctor, who may have fair concerns: in 2010, the US Institute of Medicine published new guidelines for dosages of Vitamin D which seem to discourage higher dosages. However, those guidelines are really aimed at the “worried well,” not pain patients. For more information, see own Vitamin D for Pain.
Avoid most nutraceuticals, especially chondroitin and glucosamine: they are a waste of your money

A cousin to the topic of nutrition, there are several popular “nutritional” supplements other than vitamins and minerals that people take because they are supposed to be good for your muscles and joints — the so-called “nutraceuticals.” They aren’t considered pain-killers, but people take them for pain. They aren’t anti-inflammatories, per se, but people believe they will reduce inflammation. They aren’t performance-enhancing “drugs,” but athletes and bodybuilders take them almost like drugs to enhance their performance. Nearly all supplements suffer from a serious lack of good evidence of efficacy (creatine is a notable, happy exception). Not one is a clear winner for pain, and the most famous ones — glucosamine and chondroitin, supposedly good for arthritic joint pain — are particularly suspect. They’ve been studied a lot, but even the most generous interpretations of the most positive-seeming results are still kind of underwhelming. For a thorough analysis debunking, see Vitamins, Minerals & Supplements for Pain & Healing
Despite the generally bad news, there are a couple of nutraceuticals that are mildly promising for pain and probably worth considering …
Try creatine & bromelain
Somewhere in the mess of generally disappointing nutraceuticals (see previous tip), there is probably something that works at least a little bit for someone. Creatine and bromelain are definitely not sure things, but out of the top dozen or so candidates they are the only two that I’d bet any money on — both are safe enough, cheap enough, plausible enough, and based on enough evidence to be worthwhile. (All other nutraceuticals fail on at least one of those scores.) Creatine is the most “legit” performance-enhancing nutraceutical, which really does reduce muscle fatigue — and, just maybe, some pain along with it. Bromelain, an enzyme from pineapples, allegedly has anti-inflammatory properties that are, just maybe, actually real. If you’re going to try any supplements, these are the two to take seriously.
Quit smoking: it’s not just for your lungs

Does “quit smoking” seem a bit boring for a pain-busting tip? I don’t think so. “Smoking was established long ago as a strong predictor of failure of pain treatment,” writes Dr. Tim Taylor, a chronic pain specialist. “Smokers are so difficult to treat that I will not accept smokers as patients.”
Smokers often believe that they’re mostly just hurting their lungs, but that’s just the tip of the iceberg: smoking affects practically everything, and practically everything affects chronic pain, and so there’s bound to be overlap. And there is: smokers are two to three times more likely to be in pain than non-smokers (see Smuck et al.). Smokers are compromising so many aspects of their health that quitting is a vital pre-requisite for beating pain. See Smoking and Chronic Pain.
Postural correction: difficult and usually not very important, but still …
The evidence strongly suggests that posture is not terribly important as a factor in any serious chronic pain problem. Poor posture and structural problems like a swayback (excessive lordosis) definitely do not necessarily cause pain. Meanwhile, plenty of people with acceptable or excellent posture have terrible pain problems. So something isn’t adding up there! Actually changing posture is also so generally difficult that it is probably rarely worth the trouble — I’ve never seen a single clear case of improved posture. Nevertheless, I don’t dismiss it entirely, and there are certainly some postural habits that probably create unfortunate consequences. Poor posture has got to be at least a contributing factor in some problems, and some postures are related to or confused with a more important concept: postural strain from, say, bad ergonomics (see next tip). Probably the most effective approach is simply to increase levels of complex physical activity in your life.
For more in-depth examination of the subject, see Does Posture Matter?.
Tits up! Use “power poses” to reduce pain sensitivity
It’s relatively obvious that posture is shaped by mood and all kinds of other social and emotional factors. What is much less well known is that it is a double-edged sword that cuts the other way: posture can create and reinforce emotional states! And that’s not all. If posture can change emotions, it’s no surprise that it can also change pain sensitivity. So, here’s an easy science-powered pain relief tip: Stand tall! Assume a bold, confident posture. Or, as a mentor of mine liked to put it, “Tits up!” This will actually reduce pain — a little. A temporary reduction in sensitivity is hardly a cure for chronic pain. But take it anyway! This qualifies as a good tip because it is such low-hanging fruit. For more about this idea, see the section about the emotional risks of posture in my big posture article.
Reduce postural stress with ergonomics: not just about your keyboard height
There’s poor posture, and then there’s postural stress — that is, circumstances that make it difficult to maintain a posture. People often deal with strain due to poor ergonomics: poorly designed and inherently awkward work. Ergonomic fine-tuning of your workstation and life is usually much less important than being generally active and taking regular breaks from whatever you do, however you do it. However, there are some common ergonomic problems out there that certainly need correcting, and it’s well worth looking for the ergonomic “low-hanging fruit.” The problems I’ve encountered the most often: high monitors (headaches!), holding the phone to the ear (neck cricks), and reaching high and far for keyboards and mice (elbow, wrist pain). And don’t forget that microbreaking and mobilizations are great strategies for reducing postural stress … and especially important when you can’t actually eliminate the stress.
Use a wobble cushion: an unstable recovery?
Sitting on a wobble cushion is like sitting on an exercise ball — it gives your postural musculature something to do, keeps your back and core musculature “frisky” — only it’s more practical and convenient. Sitting on exercise balls is a great idea, but they are bulky, you can’t sit on them all the time, and there is rarely room in anyone’s office for both a chair and an exercise ball. Enter wobble cushions: compact enough to be convenient, wobbly enough to be mildly therapeutic. This isn’t going to cure anything, but postural stagnancy and strain from sitting is such a loud “background noise” for so many people, and this is such a reasonable and plausible partial antidote, that it earns itself a section on this page.
See Does Posture Matter? for more.
Crunch! Self “adjust” your spine
First of all, stop worrying about cracking your joints: there is no compelling evidence that there is any significant risk in doing so. Second of all, if it’s appealing, make a point of cracking your spinal joints in moderation in order to facilitate recovery from pain and stiffness in the torso and neck. The chiropractic profession would have us believe that joint cracking is essential to general health, which goes way too far. However, scientific evidence has shown that it probably is at least a little bit helpful to stimulate joints with cracking and other “adjustment.” Obviously, please don’t crack your joints if you hate the feeling. But if it feels relieving, by all means, go for it, without guilt or concern, in reasonable doses. Like many physical therapies, it’s not “fixing” anything, but it does supply the joint and vicinity a blast of fresh sensory input which probably has a cascade of minor benefits.
I offer an incredibly detailed analysis of the science of spinal manipulative therapy to customers who purchase either my neck pain or back pain tutorials. Some simpler related information is available to all in my article The Chiropractic Controversies
The confidence cure: rational, informed confidence can probably reduce pain
Not all tissue damage hurts, and not all pain is caused by tissue damage. Pain is determined completely by the brain, after it considers many factors. Nerves send messages about problems to the brain, but the brain decides how much it matters (and even tells the nerves how sensitive to be). Thus, we invariably hurt more when we are worried, and less when we are calm. If your brain is not “worried” about a sensation, there will be no pain. A lot of chronic pain is caused by a brain that still thinks there’s a problem in the tissue. For instance, many things that look scary on an MRI of your back are actually painless in most people. Pain is not “all” in your head, but is strongly affected by what’s in your head. The most reliable way to change what’s in your head is education. Such knowledge creates a kind of “placebo,” but without the sugar pill.
This principle is of critical importance to pain management and recovery. Anxiety reduction through education needs to be a part of every difficult healing process. Continue reading on this topic with Mind Over Pain. A closely related tip: “Don’t be a pain drama queen.”
Knowledge is in every country the surest basis of public happiness.
George Washington, 1790
Be kind to your nervous system: create pleasant, safe sensory experiences
Brains set the volume on pain (see last tip), but squeezing practical advice out of that basic truth is tricky. Stress relief, the confidence cure, and personal growth are three examples, but they are all difficult. Building confidence through learning? Hard, uncertain work! Stressors and mood disorders? They can be virtually invincible. Is there anything easier you can do to convince your brain that the pain isn’t so bad? Yes!
Be kind to your nervous system. Seek comfort. Be a hedonist. When your brain is freaked out and over-interpreting every signal from the tissues, “therapy” may be more about soothing yourself and feeling good and safe than about “fixing tissues.” Pain is all about your brain’s assessment of safety. Unsafe things hurt. If your brain thinks you’re safe, pain goes down. So be “nice” to your CNS in every way that you can think of. Make your life — or a joint — feel safer, gentler, more pleasant. Do it in general ways (soak the whole system in a hot tub), but also more specifically: pleasantly stroke a sore knee, give a screaming shoulder the “comfort” of a sling for a while, or cautiously but thoroughly move a troubled joint to demonstrate to your brain that it’s okay. (See, brain? We can do this! No big deal!)
Trying to create pleasantness is a very different creative challenge than trying to reduce stress. It won’t work miracles, but you can’t really go wrong trying to make yourself feel safer and happier. See Mind Over Pain for more ideas about manipulating your nervous system.
Orthotics: slip into something more comfortable

Orthotics can be a good-bang-for-buck solution to a variety of otherwise untreatable postural problems and gait dysfunctions. On the one hand, I cannot emphasize strongly enough that things like leg length differences are much less important than physical therapists generally make them out to be. However, they can be a factor, and sometimes the stars line up and orthotics make a clear positive difference. Better still, research has shown that expensive orthotics are not clearly better than cheap generic ones.
There is one problem, though: sometimes they backfire, probably because they can be difficult to adjust to, disrupting fine-tuned postural adaptations and forcing awkward new ones. Some people find the cure to be worse than the disease.
If you do need customized orthoses for whatever reason, go with a reputable supplier. Certified pedorthists are by far the best choice. You should be quite cautious about purchasing orthotics from physiotherapists, chiropractors, and even podiatrists. For more information, see Are Orthotics Worth It?.
Do not get a joint lube job: avoid artificial synovial fluid injection

Should you get a joint lube job? Just say no! The injection of artificial synovial fluid — slippery stuff — into a joint to decrease the symptoms of osteoarthritis has been in widespread use for many years now. Considering how appealing and popular the idea is, and how common joint pain is — pain which may not even be arthritic — a warning about this stuff deserves to be a tip. Do not do it. Hylaluronic acid injection is completely washed up scientifically. A 2012 review of nearly 90 trials determined that is associated “with a small and clinically irrelevant benefit and an increased risk for serious adverse events.” Your immune system can react quite melodramatically: more swelling and pain instead of less. take-home message? Combining injections and wishful thinking is bad news. For a more detailed analysis, see Should You Get A Lube Job for Your Arthritic Knee?, or the anterior knee pain guide for even more.
Heal by growing up: sometimes sweeping personal changes will also affect pain
As science advances and mind-body perspectives on health and healing become more sophisticated and practical, we understand that pain problems are powerfully mediated by stress, self-limiting behaviours, and “emotional constipation.” Professionally, I have been in an ideal position to see how people’s quirks and habits cause, slow, and prevent all kinds of healing. Particularly for people struggling with a difficult healing process, I recommend “getting personal.” Sometimes it’s a matter of just learning new coping skills for a problem that is never going away. And sometimes people need to come to terms with the fact that years of self-sacrificial workaholism — for a common example — are actually the root cause of severe chronic pain. Usually the truth is in the middle: healing requires a complex mix of coping skills and personal responsibility. Through this kind of learning, people often find long term relief.
Of course, there are nearly infinite ways of approaching this challenge, and I’ve written about it in several ways. I get more thoroughly practical in Pain Relief from Personal Growth. Mind Over Pain covers many related “mind over pain” ideas in detail. You might also want to read Dr. Gabor Maté’s excellent book When the Body Says No. Or go straight to Haven. There is also one extremely useful personal growth tool that you can start leveraging right away: see the next tip.
General activity increase: do something, anything!

The calorie-counting stairs (click to zoom). Stairs are the most ubiquitous, accessible “gym equipment” in the world
The evidence is overwhelming: moderate exercise is not just fantastic for your body, but your mind as well. Although relief from specific sources of physical stress can be critical, overall rest is sometimes the last thing patients need. A sedentary lifestyle, like insomnia, can be a “sleeper” factor — an unsuspected and underestimated major aggravating factor in many injuries and pain problems, and particularly problems caused or complicated by myofascial pain syndrome (muscle knots). A lack of exercise or variety of activity generally impairs circulation, neurological stimulation, and the vitality that is needed for healing. Worse, it’s an irritant in itself: sitting is stressful for many tissues, for instance. An increase in activity could be an important pre-requisite and support system for healing.
Training regimens and exercise classes are fine for the athletically inclined, but if you are bit of a couch potato, those are probably the last things you want to do, and you’re doomed to failure. What, then? Basics: start walking or cycling to work, take the stairs instead of the elevator, take the batteries out of the remote, etc …
See The Trouble with Chairs for more. And keep in mind that it is easier to build strength than you think.
Blow off steam: breathe and shake stress away
Despite my evolution from New Age flake to a man of science over the years, I still think this is a fascinating and useful approach to rehabilitation. Mostly it involves breathing quite quickly and deeply for up to a quarter hour, without controlling or “shaping” the movement of breath. Optionally, you can throw in a bunch of vigorous movement as well. But why?
Psychological stress aggravates pain, and it’s well worth reducing stress if you possibly can. Slow deep breathing is a classic way to tackle that, but the last thing I want to do when I am really stressed out is slow down and take a really deep, slow breath: I want to scream and huff and puff and run around in little circles! So I do! Slow breathing and chill out time can come later, after you’ve blown off some steam.
Stress is expressed in the body in amazingly strong habitual muscular tension and breathing patterns (among other things). One of the quickest and easiest ways of de-stressing is simply to mess with those patterns: to more literally “blow off steam” with vigorous breathing exercises, and (optionally) with movement, dancing, shaking, and vibration. This gets to the heart of the matter much more directly than any relaxation exercise, and provides more opportunity than athletic exertion to work with under-expressed and repressed feelings of anger, sadness, frustration, and anxiety.
For more about blowing off stream with breathing, see The Art of Bioenergetic Breathing.
Don’t be a pain drama queen! Tear up that one-way ticket to hell
“It feels like a jagged, flaming, poisoned sword ripping through my body over and over again.” People in pain really talk like that! Beware of colourfully hyperbolic description and mental imagery about pain. Patients are often tempted to dramatize the pain to make it seem more real to doubting doctors and loved ones, but it’s a trap! Before you know it, you’ll believe your own story. When you exaggerate and dramatize your pain, you directly exacerbate the neurological end of the chronic pain problem (see also The confidence cure). Dial it down instead. In fact, as much as possible, consciously do the opposite: minimize your pain, embrace stoicism, and visualize how someone you admire would cope. Say, “Doctor, the pain is 7 on a scale of 10. Sometimes probably a little more, but I try not to exaggerate it.” As long as you don’t inflate the numbers, using a pain scale is a good way to be less of a pain drama queen. See Mind Over Pain for a longer version of this tip.

“I am experiencing a disturbing amount of pain. I might actually be dying. Please help.” — #8 on Allie Brosh’s hilarious illustrated pain scale
Exercise classes: aerobics, yoga, Pilates, taijiquan, boot camp, etc …
Sometimes the goal of healing is to get to a point where you can actually think about doing a yoga class — and sometimes a yoga class is how you heal. There are many circumstances where I recommend exercise classes, usually yoga, and sometimes Pilates, taijiquan, aerobics, or cross-training classes the currently popular CrossFit or “boot camp” classes. Of course, nearly any kind of exercise, even a sport, can become a useful part of a rehabilitation program, but I have a specific reason for singling out exercise classes, especially yoga: for non-athletes who might not otherwise be interested, there is simply no better way to explore body awareness and safely test your limits with a variety of new challenges. Also, I believe that a social environment is helpful to most healing processes: seriously, injury loves company!
And yoga is not for everyone. The reputation and popularity of yoga and meditation is immense, almost oppressive, sometimes eclipsing other options. People feel that they “should” try them in order to reduce stress and contribute to a healing process. They often feel guilty for not trying them or for not liking them. If this is you, please read The Tyranny of Yoga and Meditation
Take a deep breath (because it really is good for you)
“Take a deep breath.” Really. Deep breathing is a bit of a cliché, and it will put off some readers. But many clichés ear their status fair and square, and deep breaths have clear neurological benefits that are low-hanging therapeutic fruit for most chronic pain patients. Everyone knows deep breathing is allegedly soothing, but few know exactly why.
The human body is constantly juggling stimulation and relaxation, even on a moment-to-moment basis. These phases are mediated by the sympathetic and parasympathetic divisions of the nervous system respectively, whole classes of nerves that trigger rest and repair processes. And the parasympathetic nervous system activates a little bit with every single exhalation — which is why relatively longer exhalations produces measurable relaxation.
So don’t just breath deep: inhale deeply and then exhale relatively slowly. Do that a few times and you will relax a bit. “It’s science!” And it’s good for chronic pain in a bunch of ways. This is basically the only guaranteed, universal way to conveniently, quickly, measurably calm your nervous system.
Progressive training: break up the challenge into baby steps
Progressive training is a (really) basic concept in athletics and injury rehabilitation — so basic that it seems almost unnecessary to spell it out. Yet I routinely see people failing to respect the principle of “baby steps”! The idea is to break challenges up into small intermediate goals. All serious athletes train progressively, because it’s the only way to get the job done. It is the basis of every running group. Runners who patiently increase the length and intensity of their runs are training progressively, and are at much lower risk of injury. The principle is the same whether you are fit and working towards an athletic goal, or injured and simply trying to get back to normal.
For more information, see Progressive Training.
Friction massage (for tendinitis only)
Friction massage is a specific technique applicable mostly to tendinitis. It is a method of generating carefully dosed healthy “stimulation” of connective tissues when normal use of the tendon will only aggravate the problem. Rub back and forth across the most painful spot on the tendon for five minutes, increasing the intensity whenever the sensation fades. If it doesn’t fade, stop. Frictions are not particularly evidence-based, but they do make sense; they may help either by training the tissue to be less sensitive neurologically, or by kickstarting stalled healing processes. In any case, it is easy and free to try, and quite harmless if you don’t go overboard — clearly worth a shot for such a common problem. One important caution, though: don’t do this with fresh, new cases of tendinitis, which mostly need rest.
For more detail, see Deep Friction Massage Therapy for Tendinitis.
Pain-free ROM exercises after injury: use it (thoroughly) or lose it
“Early mobilization” is an important concept in rehabilitation that dates only to the 60s — prior to that it was typical to immobilize injured patients for long periods — and has since been proven to speed healing from traumatic injuries. Even when an injury is acute (fresh), it is important to use whatever pain-free range-of-motion (PF-ROM) you have got. It stimulates circulation, metabolic activity, and normal neurological function. At the same time, of course, you have to be cautious not to irritate the injury — that’s why it’s pain free. Chronic and non-traumatic injuries and dysfunction may also benefit from more thorough mobilization, although the approach is a little different.
For more detailed information, see PF-ROM Exercises. The next tip about “mobilizations” is closely related, but the difference is that with PF-ROM you avoid all tissue stress, but with mobilizations you graduate to more vigorous stimulation.
Mobilizations: massaging yourself with movement
“Mobilizations” are rhythmic, repeated movements that alternately stretch and contract musculature and other soft tissue — massaging your tissues with movement. I prescribe at least one or two key mobilizations to nearly every client, usually in preference to stretching. Mobilizations are more “neurologically interesting” than stretching and stimulate more metabolic activity in the tissue while remaining gentle. They are more practical and efficient than stretching in many ways, especially because they can affect more tissues more quickly, and because they constitute both a better warm up and a better warm down for more intense activity. Mobilizations are a particularly helpful thing to do while “microbreaking” — taking frequent short breaks from a stressful or sedentary working position.
See Mobilize! for more information.
Don’t bother with hip strengthening: “weak hips” is a poor scapegoat for chronic leg injuries
Hip weakness or “dead butt syndrome” has become the most popular new scapegoat for all the common athletic overuse injuries below the waist (especially running injuries, like iliotibial band syndrome, patellofemoral syndrome, shin splints, and The Complete Guide to Plantar Fasciitis). It’s being blamed so often that warning people about it seems worthy of this list. Simply put, the evidence is not in — and, indeed, what little evidence there is has been blown way out of proportion. If you want stronger hips just for the sake of stronger hips, knock yourself out: just keep your expectations low. No way is it a magic bullet. It sounds too good to be true … and it is.
It’s a complex subject, but that’s what this website is all about! You can read all about it, in excruciating detail: Does Hip Strengthening Work for IT Band Syndrome?.
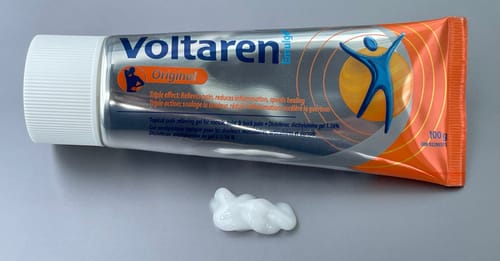
Try Voltaren: anti-inflammatory medication only where you need it
Voltaren® is a useful rub-on anti-inflammatory medication (topical diclofenac). It’s proven effective and FDA-approved for osteoarthritis, and it probably also works for some other kinds of common body pain. The topical form means that dosing is minimal, targeted, and much safer than oral diclofenac. See Voltaren Gel: Does It Work? The science of the topical pain-killers, which can be effective without dosing your entire system.
The most popular of all “herbal” pain creams has precious little herb in it
One of the most popular pain-relief products of any kind, homeopathic Arnica montana — Traumeel is a popular brand — is not very herbal. Homeopathic remedies are extremely diluted, so the actual amount of arnica is mind-bogglingly small — in fact, well below what is considered necessary to be chemically active. If it worked, it would be easy to prove — but it never has been proven by the standards we expect of other medications. Homeopaths often argue that science can’t test the effectiveness of homeopathy because it’s beyond our understanding, but that’s not true: you can always test if something works (even when you don’t know how it works).
If a highly diluted arnica cream is in your medicine cabinet, you should reconsider whether or not it belongs there. For more information, see Does Arnica Gel Work for Pain? A detailed review of popular homeopathic (diluted) herbal creams and gels like Traumeel, used for muscle pain, joint pain, sports injuries, bruising, and post-surgical inflammation.
Check your drugs! Pain can actually be a side effect — even of pain killers!
Anyone struggling with stubborn pain should be aware that pain may be related to medications. For instance, pain is a side effect of a popular class of drugs for osteoporosis, the Bisphosphonate (Wikipedia), which can cause “severe and sometimes incapacitating bone, joint, and/or muscle pain” which “may occur within days, months, or years” after first taking the medication. If you are 40+ and grappling with a mysterious pain problem, check your medicine cabinet for bisphosphonates in particular, but of course any other medication that could cause pain as a side effect.
The statins — cholesterol lowering drugs like Crestor and Lipitor — are another example of a common drug with a possible pain side effect: “The most common statin side effect is muscle pain” (Mayo Clinic). On the other hand, this is controversial: in a 2017 study, statins didn’t boost muscle risks in patients unaware they were taking them (Gupta et al.).
Even ordinary pain-killers themselves may actually lead to more pain over time, if you take quite a lot of them, through an effect known as “analgesic rebound.” Your body gets used to the drug supply, so it dials down its own pain-management systems. You can end up feeling more pain when you reduce your intake. This can be a subtle vicious cycle that can go on for years without being particularly obvious — just routinely making things a little worse.
This is very much a “talk to your doctor” kind of issue, so there’s little additional about it on this website, but see 38 Surprising Causes of Pain for more detail about some drugs, and many other ideas about possibly surprising origins of pain.
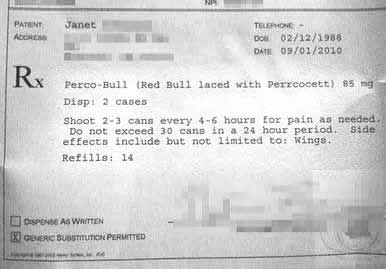
Best prescription ever?
“Perco-Bull (Red Bull laced with perrcocett) [sic]… Side effects include but not limited to: Wings.”
Master over-the-counter pain medications
Over-the-counter (OTC) pain medications are fairly safe and somewhat effective in moderation and work in different ways, so do experiment, but do it cautiously. There are four kinds: acetaminophen/paracetamol (Tylenol, Panadol), plus three non-steroidal anti-inflammatories (NSAIDs): aspirin (Bayer, Bufferin), ibuprofen (Advil, Motrin), and naproxen (Aleve, Naprosyn). Don’t take any of them chronically — risks go up over time, and they can even backfire and cause rebound headaches. They are all probably equally effective for acute injuries (Hung), but benefits vary with people and issues (chronic pain, headaches, arthritis, etc), and relief is usually minor at best.
Acetaminophen is good for both fever and pain, and is one of the safest of all drugs at recommended dosages, but it may not work well for musculoskeletal pain (at all?), overdose can badly hurt livers, and it might harm fetuses. The NSAIDs all reduce inflammation as well as pain and fever, but at any dose they can cause heart attacks and strokes and they are “gut burners” (they irritate the GI tract, even taken with food). Aspirin may be best for joint and muscle pain, but it’s the most gut-burning of them all. Voltaren is an ointment NSAID, effective for superficial pain and safer (Derry). Athletes, puh-lease don’t take “Vitamin I” to prevent soreness — it doesn’t work! Worse, it may impair tendon and bone healing.
For more information, see The Science of Pain-Killers.Get in the pool for pain
Anyone with almost any kind of chronic pain should seriously consider spending more time in the pool (doing almost anything, but aquajogging is a particularly good choice). Immersion and flotation have curiously potent effects, particularly partial relief from gravity, which makes movement feel easy, cushioned, and safe — and feeling safer with movement can be a critical stepping stone in all kinds of rehabilitation and pain management. Modern pain science makes it extremely clear that pain is an expression of perceived danger, and water is one of the few places where we can both be more active while also actually feeling safer — a precious combination.
The pool isn’t for everyone, and there are some downsides, like getting chilly (a deal-breaker for some chronic pain patients). However, it is well worth taking a shot at it and making the effort to make it work for you. Read more: Get in the Pool for Pain.
Relaxation massage: not just fluffy
Relaxation massage has an unfair reputation for being “fluffy” and unimportant, when in fact its potential value is rather obvious in light of how the nervous system works: pain makes us more sensitive to pain, while pleasant and safe sensory experiences help to break that cycle. Well, a good quality relaxation massage is just about the most pleasant and safe sensory human experience there is! (It is literally “better than sex” in many ways. Sex is too emotionally complex for it to be routinely “soothing” for anyone but stable couples.)
The soothing power of touch is often regarded as a sort of “nice bonus” or sensory gravy in massage therapy. But it’s the main thing. Maybe the only thing. Alas, relaxation massage is often denigrated by massage therapists who want to seem more like physical therapists with “technical” massage skills. So it’s tricky to find good quality relaxation massage: artful, satisfying, neither too shallow nor too rough. It’s also fantastically expensive and rarely insured, a health care luxury. And it’s unclear that it has any significant, lasting benefit for pain patients. Very little is proven here. However, we do have good confidence that touch has a number of effects on the CNS that are at least valuable, if not “curative.”
Novel sensory input: change how it feels with taping, bracing, or other tricks
Got a hurt? Change something — almost anything! — about how the area feels. Make it feel as different as you (cheaply) can. Pain is tuned by the brain based on many factors. Sensation is one of those factors. If you can make a body part feel significantly different in any way, it may help — but especially if you can make it feel safe, protected, stabilized. In fact, this probably explains why many treatments for pain problems are popular despite having underwhelming results. Classic examples: taping, bracing, strapping, splinting, salving, vibrating, heating, icing. Regardless of how they supposedly work — there are many overly complex explanations — most of these methods mostly just change how a body part feels.moreObviously bracing a knee with a ruptured ligament is a different case, and straighforward. Similarly, you can certainly tape up a sprained ankle for pure stability — which is not a sensory effect. But bracing is often prescribed for much less clear reasons, and taping gets even weirder, like the absurd colourful tape that was so faddish in the 2011 Summer Olympics. These approaches to rehab often have wildly speculative rationales, when most likely they are all just creative ways of changing sensation.
The benefit of novel sensory input is probably not much more profound than being distracted by a loud noise … but we can add it to the treatment toolkit, with reasonable expectations. If you have a hurting body part, by all means change how it feels using any cheap, convenient, creative method — there’s little reason not to.
Don’t knock “masking” symptoms
“Masking symptoms,” especially with medications, is often maligned because it doesn’t “treat the root cause.” But masking symptoms can be a good idea, and it should not be eschewed just because it doesn’t have a real healing effect … because there are very few real healing effects! “Healing” is mainly about removing impediments to natural recovery, like stress on tissues. It’s not dictated by some mythical power to speed healing, but by a strong understanding of the nature of the problem and what pisses it off and impedes recovery. Focus on facilitating natural recovery, and don’t knock a little “symptom relief” along the way. See Masking Pain is Under-Rated: “Masking” symptoms is often scorned, but sometimes symptoms need masking — especially pain!
Marijuana is worth trying, especially for neuropathic pain
There is “substantial evidence that cannabis is an effective treatment for chronic pain in adults,” according to a major report produced by the National Academies of Sciences, Engineering, and Medicine in early 2017. However, that is probably overstated, because “very little is known about the efficacy, dose, routes of administration, or side effects of commonly used and commercially available cannabis products.” Other reviews of the science, focused just on pain, have been much less encouraging, warning that there’s just not enough evidence about any kind of chronic pain, not even neuropathic pain, and especially about CBD specifically (as opposed to THC).
Cannabis probably isn’t going won’t work miracles in most people, but it may help, and it’s quite safe, though not entirely. The major safety concerns are the risk of frightening side effects from accidental overdose (not very dangerous, but highly alarming, like panic attacks); a bizarre vomiting disorder called cannabinoid hyperemesis syndrome; and there is an on-going controversy about a risk of causing psychosis (mostly in younger people consuming a great deal and likely with underlying vulnerability).
Beginners should mostly avoid edibles (awkward and unpredictable dosing) and consider vaporizing rather than smoking.
Part 3
Appendices
Related Reading
This article is chock-a-block with links to other relevant articles, elaborating on the tips. But here are a few other articles that also provide a high-altitude view of pain and injury troubleshooting:
- “Seven Pathways For Getting Out of Pain,” Todd Hargrove, BetterMovement.org. This is a nice collection of tips from Todd Hargrove, a Seattle Rolfer and writer with a real knack for simplifying and synthesizing complex ideas.
- Vulnerability to Chronic Pain — Chronic pain often has more to do with general biological vulnerabilities than specific tissue problems
- Mind Over Pain — Pain can be profoundly warped by the brain, but does that mean we can think the pain away?
- Popular but Weird & Dangerous Cures — The most dangerous, strange, and yet popular snake oils and “treatments” in history (and why anecdotes and testimonials cannot be trusted)
- 38 Surprising Causes of Pain — Trying to understand pain when there is no obvious explanation
What’s new in this article?
2019 — New section: No notes. Just a new chapter. [Updated section: Reduce vulnerability to chronic pain.]
2018 — New section: No notes. Just a new chapter. [Updated section: Take a deep breath (because it really is good for you).]
2018 — New section: No notes. Just a new chapter. [Updated section: Be aware of sneaky causes of pain.]
2017 — Added bonus tip: Muscle clenching has been shown to reduce pain sensitivity (Smith et al.) — a good additional reason to challenge muscles. [Updated section: Strength training: better, easier than you thought.]
2017 — Science update: Cited another new review (Nugent), more focused on pain, that tempered my enthusiasm a bit. The tip stands, but not as tall. [Updated section: Marijuana is worth trying, especially for neuropathic pain.]
2017 — Abridged: Made the summary more concise, now that there is a featured article for aquatic therapy. [Updated section: Get in the pool for pain.]
2017 — New section: Marijuana finally makes it to the tips page! Overdue, but the evidence is good enough now. [Updated section: Marijuana is worth trying, especially for neuropathic pain.]
2017 — Removal: Got rid of advice to buy fancy “ergonomic” chairs. I no longer believe it’s good advice, because back pain is not linked to sitting too much.
2016 — Minor addition: A note about aquajogging. [Updated section: Get in the pool for pain.]
2016 — Revised: Integrated a near-duplicate section and updated the language a bit. [Updated section: Blow off steam: breathe and shake stress away.]
2016 — Edited: Clarified a key concept: the methodology of self-treatment experimentation. [Updated section: Introduction.]
2015 — Adjustments: Small but meaningful improvements regarding safety and efficacy. [Updated section: Master over-the-counter pain medications.]
2015 — New: [Updated section: Master over-the-counter pain medications.]
2015 — Minor update: Added statins. [Updated section: Check your drugs! Pain can actually be a side effect — even of pain killers!]
2015 — Minor update: Made the tip more concise, and linked out to a new short article about smoking and pain. [Updated section: Quit smoking: it’s not just for your lungs.]
Archived updates — All updates, including 30 older updates, are listed on another page. ❐