Mobilize!
Dynamic joint mobility drills are an alternative to stretching, a way to “massage with movement”

Use it or lose it! (But you don’t have to be able to kick as high as your head.)
Mobilizations are rhythmic movements that “massage” your muscles and joints with movement — wiggle therapy. Mobilizations involves a lot of moving a joint through its range, without resistance. It’s just extremely easy exercise, basically, which is why it has a role to play in rehab.
The most widely accepted term for this kind of exercise is “dynamic joint mobility drills,” and they can also be considered “dynamic stretching” (but that stretches the definition of stretching1). But I prefer mobilizations, or just “mobes,” because that’s what I spontaneously called them early in my career as a Registered Massage Therapist, when I was teaching mobilizations in an exercise class at Sunset Beach in downtown Vancouver. Nostalgia!
“Mobes” can warm you up gently, gradually expand your comfort zone, relieve tension and perhaps muscle knots, and facilitate healing. Mobilizing is an extremely easy form of therapeutic exercise, easily fine-tuned for anyone, which can be used to efficiently stimulate specific tissues with just the right amount of activity — not too much, but enough to facilitate healing. “Motion is lotion,” as the old rhyme goes.2
A great deal of scientific evidence suggests that movement in general and “early mobilization” in particular is a valuable part of recovery from injuries and surgeries — or at least not any kind a problem. This flies in the face of the idea that we need to be immobilized to recover from injury.3 I also recommend mobilizations for:
- Chronic pain syndromes such as fibromyalgia, sensitization, and myofascial pain syndrome.
- A wide variety of so-called stubborn “injuries” or pain problems — such as low back pain, neck pain, headaches — which are routinely caused or complicated by myofascial trigger points.
- As an alternative or supplement to popular therapeutic stretches of dubious value, like IT band stretching for runner’s knee, or wrist stretches for carpal tunnel syndrome.
- Prevention of injury due to sports, inactivity, or the combination (weekend warriorism).
- Fitness facilitation for elderly patients who are struggling to stay active.
These applications are all unconventional and generally unproven, although the rationale is sound and the exercises are free and safe. In this article, I will explain why you should mobilize, and of course how.
Motion is lotion.
timeless wisdom
The origin and ultimate reason for the brain’s existence is not to help us think or feel or create art, but to control the movement of the body.
Todd Hargrove of BetterMovement.org, nicely paraphrasing Daniel Wolpert’s TED talk, The Real Reason for Brains
Early mobilization — a critical rehab concept
In 1966, in Vietnam, my father was shot in the leg, a terrible wound that shattered his femur from hip to knee. A progressive young doctor insisted that he start walking as soon as the bone could take it — a direct contradiction to the orders of a more senior physician, a doctor who was actually famous for inventing the traction equipment my father was strapped into. My father followed the younger doctor’s advice, and experienced a remarkable recovery. We can never know for sure if early mobilization was as decisive a factor for him as it seemed to be, but for the last thirty years orthopaedics has evolved decisively in that direction. Today, doctors often won’t put a cast on a fracture if they can avoid it — fractures heal faster when they aren’t completely immobilized.45
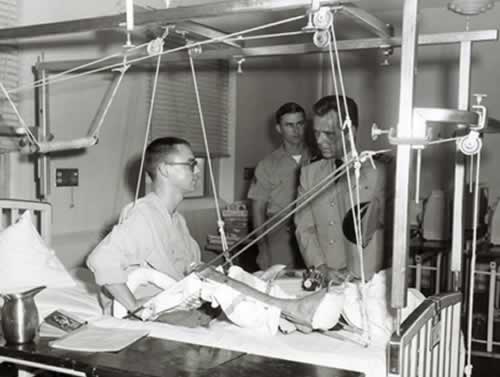
My father in traction
After a bullet shattered his femur, a young physician encouraged my father to get moving as soon as possible. Here he is visiting with actor Jackie Cooper. Early in the war, Vietnam veterans were treated like heroes.
Acute low back pain has been shown to respond much better to normal activity than to bed rest.67 Achilles tendon ruptures have been shown to heal faster with early mobilization after surgery.8 Whiplash victims recover much faster if they get moving right away after their accident, rather than wearing a collar.9
For all the evidence that early mobilization is a crucial concept in rehabilitation, the prescription is easy: just do as much as you can, as soon as you can, and let the pain be your guide. It’s not a type of exercise, just a sensible idea, no different than it was in 1966 — it’s just “let’s get you moving as soon as possible.” It didn’t seem like common sense forty years ago, when “bed rest” was the first thing physicians recommended for practically everything, but it does seem straightforward these days.
Bourne concentrated on rest and mobility. From somewhere in his forgotten past he understood that recovery depended upon both and he applied rigid discipline to both.
The Bourne Identity, by Robert Ludlum, p. 137
Mobilizations are good for prevention, too!
Mobilizations aren’t just for rehab — they are also good for keeping you from needing rehab in the first place!
For one athletic season, over a thousand female footballers — that’s “soccer” to many of us — participated in a warm-up routine.11 Their goal was to “improve strength, awareness, and neuromuscular control” — coordination practice, basically. Many of the exercises were similar in principle to the kind of mobilizations I teach.12
Several hundred other players did no such exercises.
The difference between the groups was remarkable. The athletes with the coordination-o-centric warm-up had fewer traumatic injuries, and fewer overuse injuries, and the injuries they did have were less severe. This evidence strongly suggests that mobilizations specifically are generally a useful tool for preventing athletic injury. Another large project led by the same scientist, published a couple years later in 2010, found that “the risk of overall and acute injuries was reduced by more than a third” by good participation in a warm-up program,13 specifically the 11+ warm-up regimen recommended by FIFA — more intense than mobilizations, but otherwise quite similar in spirit.

Massaging with movement
Mobilizations as a therapeutic exercise system are best understood as “massaging with movement.” That phrase neatly summarizes most of this article. Feel free to skip down to the practical sections now, if you don’t need to read all the details. “Active stretching” or “dynamic stretching” is a similar concept.
Mobilizations are an easy, cheap, safe, efficient way of stimulating tissue — and stimulating tissue has many benefits. I prescribe mobilization exercises extensively to treat just about all kinds of pain problems, even in cases of pain where there is no reason to expect any significant relief by any method. Mobilization is still useful, I think, even then.
Unfortunately, there is little direct scientific evidence to support that opinion, although I suspect that it will emerge steadily over the next twenty years. Evidence is already emerging around the edges. Just as it is now more or less established that early mobilization is an important part of rehabilitation, it will probably also be established that it is more broadly beneficial. For instance, if you do mobilizations, to some extent you are also doing a kind of therapeutic exercise recommended by many physical therapists, neural mobilization, which is similar in spirit but more specific.14
Meanwhile, a sound rationale will have to suffice … and the indirect evidence. And both are pretty good.
The Goldilocks principle

We know from research that regular moderate activity is generally a good thing,1516 tissue stagnancy is bad news, and that overexertion is dangerous to healing tissues.17
That pretty clearly implies a need for some kind of in-between exercise intensity, something not too easy nor too hard, but a Goldilocks “juuuust right.”
But conventional therapeutic and rehabilitative exercise tends to hit only the extremes. For serious injuries, there are the gentlest of exercises, such as pain free range of motion (PF-ROM) exercises, like dangling and swinging your arm in a six-inch circle when you’re recovering from a shoulder dislocation. That’s your only option when you can barely move your shoulder. But what if you have more or less normal use of your arm, but have nevertheless had chronic, nasty shoulder pain for three years?
That’s when your physiotherapist will almost inevitably prescribe endurance or strength training exercises — which are often too intense, and aggravate the problem or simply don’t help it, even while your continuing difficulties are interpreted as a sign that you “really need” the exercise. What you “really need” is a compromise. You need mobilizations! This is where they fit into the scheme of rehabilitative exercise:
| Repetitions | Loading | |
|---|---|---|
| PF-ROM Exercises | 50–100 | negligible |
| Dynamic joint mobility drills | 30–80 | light, very easy |
| Endurance Training | 12–50 | moderate |
| Strength Training | 6–12 | moderate to high |
Mobilizations fill in the gap in conventional rehabilitation exercise between PF-ROM and endurance training. They are ideal for a wide range of patients, the neglected masses of people who are not exactly acutely “injured,” but not exactly feeling good either:
- people with injuries that have turned into chronic pain problems
- people with muscular pain and stiffness that has reached disabling intensities, and is eroding quality of life without ever having sustained an “injury”
- people with mysterious widespread pain
- people who are in pain from a lack of activity, such as chair warriors, the elderly and infirm, and those with other serious injuries or disabilities
These are enormous groups of suffering people for whom PF-ROM may be too gentle and endurance training too much.
Obviously, if you don’t exercise at all, it is not good for you. Exercise improves your health. And a lot of exercise improves your health a lot. But that doesn’t mean that insanely large amounts of exercise are insanely good for your body. At some point, too much begins to damage various physiological systems. Everything in physiology follows the rule that too much can be as bad as too little. There are optimal points of allostatic balance.
Why Zebras Don’t Get Ulcers, by Robert M Sapolsky, 123
Sick muscle syndrome
Muscle pain is an extremely common human experience. Still a medical puzzle, we call spots sensitive, tight-feeling muscle “knots” or “trigger points.” They come up all over PainScience.com because it’s safe and cheap to experiment with self-treatment, often worthwhile, and also because muscle pain has an exasperating tendency to “get involved” in many other painful problems. More specifically, trigger points may cause, complicate, and/or replace other pain problems. And yet doctors and physical therapists of all kinds tend to be unaware of the potential clinical significance of muscle. So it’s a nice opportunity for helpful public education.
I have a book all about muscle pain, so see that for (a lot) more information. But it’s important to say a few words about it here, because mobilizations and muscle knots were made for each other.
I call myofascial pain syndrome “sick muscle syndrome,” because muscle knots are a muscular dysfunction that makes muscles weak and quick to fatigue. They ache and feel kinda gross. Overstimulation or overexertion in the form of strength training, endurance training, or even stretching can either help or irritate them, and it’s impossible to predict.18 And yet they will also typically be aggravated by stagnancy. Life in a chair, for instance, may be one of the primary causes of myofascial pain syndrome.19
For most people with pain, most of the time, it makes sense to compromise with a mild to moderate exercise intensity (Goldilocks principle), and also to work with a good variety of movements — not too much of any one thing. Mobilizations to the rescue! Mobilizations are a great way to work cautiously through muscle pain — or at least to get some tolerable exercise while afflicted.
It is simply unknown if a lot of mild-mannered contraction actually “fixes” muscle pain, but it certainly might. Even if it doesn’t, it is still a sensible coping activity — the best you can do in a bad situation.
How to do mobilizations
Mobilization exercises are easy to invent for yourself! One of the main reasons that I am enthusiastic about mobilizations is that nearly anyone can do them with only a small amount of instruction.20 To create a mobilization exercise, you need the following elements:
- the full range of movement of a joint, or multiple joints
- muscles lengthening and shortening
- easy and almost painless motion
- lots of repetition
Mobilizations depend on movement to get the job done. Choose a joint, perhaps one closest to the pain if your pain is in a specific location, and begin to explore its range of movement. Which directions can you move it? How far? See, you’re already mobilizing!
Start to move back and forth in the joint’s range. Visualize the muscles attached to it: are they shortening and lengthening? The muscles do not have to contract hard, but they do have to contract, enough for metabolic activity. Imagine the muscle being squeezed out like a sponge every time it contracts. Picture the bones “stirring” your muscles.
Is it easy? If you are injured or in pain, usually there is some limitation to the movement. Find the “edge” of your range. Approach your limits, feel the edge, and retreat. You don’t have to test it hard. Achieve results with repetition, not intensity.
How much repetition? Quite a lot …
Repetition, repetition, repetition, repetition, repetition, repetition, repetition …
The real power of mobilizations is in the repetitions. Every repetition of a movement is like a message to the body, asking it to function, to do its job, to learn how to move like that and be okay with it. The message is mild-mannered, but persistent. Repeat it enough, and the body will start to respond. Most pain and stiffness will yield sooner or later if you just … keep … asking.
How many times should you repeat the exercise? Lots. Enough that you should be thinking, near the end, “Wow, this is really quite a lot of these.” Once you have found a satisfying movement, you should repeat it approximately 25–75 times in a single set, and you should do approximately 1–3 sets per day. For example:
- a patient with an acute neck crick might perform neck circles 25 times in each direction, for a total of 50 per set, two sets per day, for three days
- a patient with severe chronic low back pain might do lumbar flexions and extensions 50 times in each direction (50 flexions, 50 extensions), for a total of 100 per set, once per day for three weeks
- a patient with fibromyalgia might do smaller sets of 20 repetitions of several different mobilizations in one workout, once per day, every day forever
There is one really important thing to avoid with repetitions: don’t try to split up a large batch of mobilizations into pieces over the whole day. Remember, every movement is like a message to your tissues. The message must be repeated, or the body seems to “forget” what you were asking for. If you split your mobilizations up into three smaller batches at breakfast, lunch and dinner, then your body won’t get the message at breakfast, won’t get it again at lunch, and still won’t get it at dinner. The purpose of the exercise is to “learn” the movement — to learn that it can be done without pain, in particular — and that learning process probably requires some concentrated exposure to the stimulus, for the same reasons that a piano student who practices for a single 20-minute session per day is probably going to learn better than a student who does a bunch of 2-minute sessions per day.
Of course, unlike a suffering piano student, you’re perfectly free to listen to music or have the TV on while practicing … 😃
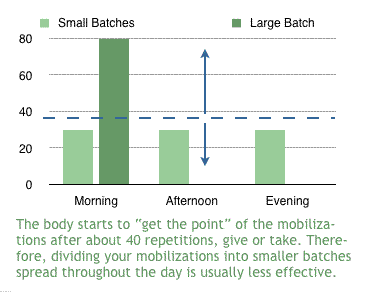
Very generally speaking, most people’s bodies don’t seem to start to respond to the “message” until somewhere between 25–50 … and definitely on the higher end of that for older and more severe problems.
Troubleshooting: make it easier!
A common mistake is to give up instead of just making it easier.
If mobilizing feels exhausting to your muscles, make it easier.
If you start to tighten up, make it easier.
If it hurts too much, make it easier.
Make it as easy as necessary to allow lots of repetitions! If you’ve tried this and a mobilization still feels like a Bad Thing in any way — or just pointless — then please listen to your instincts and stop. Mobilizations aren’t good for every situation, just most of them.
Trust your instincts (or “The Squirming Method”)
Although a knowledge of anatomy is required for cooking up the very best mobilizations for certain problems, most worthwhile mobilizations are obvious, intuitive, almost instinctive.
The body abhors stillness.21 Most of us tend to start mobilizing by instinct. Everyone squirms when they are uncomfortable, when we’ve been sitting for too long. Wrenching the neck or rolling the head in a circle, swinging the arms, opening the chest in the morning, swinging the hips, a quick toe touch … these are all common, natural “mobilizations.”
But these movements tend to be brief, and are often negative, even desperate if you are in chronic discomfort. Instead of mobilizing, people try — often unconsciously — to squirm, wriggle and wrench their way free of pain and stiffness. They rarely do more than take the edge off, at best.
To convert these anxious movements into therapeutic mobilizations, simply make them more deliberate, positive, and thorough. Don’t just pull your neck to the side once or twice: do it ten times, or a hundred times. Convert the instinct into an exercise! Watch for how you tend to squirm, and use it as the basis for a mobilization.
| Squirming | Mobilizations |
|---|---|
| instinctive | rational |
| desperate | optimistic |
| takes the edge off | therapeutic |
| 1–3 repetitions | 10–50 repetitions |
Use your favourite stretches as inspiration
Mobilizations are probably more therapeutic than stretching. Todd Hargrove puts it well:
Joint mobility drills have several advantages over static stretching. First, they involve movement, which is good, because you probably want to get better at moving, not just staying still with your limbs splayed out. Second, most of the work in a static stretch is done at end ranges of motion that don’t get used very often. By contrast, joint mobility drills usually involve movements through the middle ranges of motion where most of life and sport occur. So they promise to have more applicability to real world tasks. Healthy athletic movement at most joints has far more to do with quality of motion than quantity of motion.
But let’s not throw the baby out with the bathwater. If nothing else, your favourite stretches are a good source of inspiration: any stretch can be converted into a mobilization simply by entering and leaving the stretch rhythmically.
People tend to “accidentally” mobilize when they meant to stretch anyway: impatient with slow stretches and craving the stimulation of more movement, stretchers often hold their stretches only briefly, and then repeat them haphazardly trying to “scratch the itch” of stiffness. All that is needed to turn this kind of stretching into a more effective mobilization is simply to make it more rhythmic and deliberate. You can even think of mobilizations as a kind of stretching, or as “dynamic stretching.”22
And, of course, static stretching may have some value as well. It’s a bit dubious, but holding a stretch often feels so good that I recommend including it in your mobilizations. Simply pause the mobilization in a stretched position for as long as you like, and then resume moving when you are ready.
But bear in mind that classic slow or static (still) stretching is physiologically boring — not much happens. Indeed, evidence and reason show that stretching cannot achieve the goals that people usually have in mind for it.23 It is possible that stretching may be useful for relieving some stiffness and pain caused by trigger points, but probably not much in most cases.24
Meanwhile, mobilizations are more stimulating, and almost certainly affect more tissue, more efficiently. They probably have both significant general benefits, as well as a more direct effect on trigger points.
Not a life sentence
Mobilizations aren’t into “commitment.” They’re great — but partly they’re great because you don’t have to take them too seriously. The goals are relatively modest, so it’s not all that hard to achieve them. Precision and discipline need not apply.
That’s quite different from the physical therapy standard, which tends to be rather heavy-handed: multi-week recovery regimens that often take pages to outline and a substantial commitment that almost anyone would consider tedious, and few people can actually stick to …
| 1–5 exercises | 3–20 exercises |
| a few minutes per day will do it | commonly at least a 30-minute daily commitment |
| a few days is usually sufficient | several weeks of regular exercising is often considered normal |
| not a life sentence | kind of feels like one … |
The advantage of mobilization is that it is relatively easy to prescribe just a few relevant exercises that efficiently address the tissues in need. And there is little need to do them without knowing if they are doing any good: the benefits should be reasonably obvious within three days at the most. If there are no obvious benefits, just let it go. (If the benefits are obvious, it won’t matter much to you whether it takes three days or three weeks.) But in any case, mobilizations generally shouldn’t be continued for long. They should be performed in relatively concentrated batches as needed — whenever you feel like it, and until you feel done.
Unless, of course, you just like them …
Mobilizing for pleasure … and prevention
Like stretching, mobilizing just feels good, and mobilizing regularly is an ideal way to maintain musculoskeletal health as well as restore it. A set of your favourite mobilizations can easily be the meat of a pleasing daily regimen — like a little yoga ritual, but more dynamic and less about stretching, or like taijiquan but without all the tradition and demanding technique.
Mobilizations are most of all like qigong, Chinese “calisthenics,” but are much more Western in style: practical, efficient, “just do it.”
If you’re not actually trying to fix something, mobilizations do not have to be done in large batches. “Small batch” mobilizations are more useful for maintenance and prevention, primarily because you can quickly do a wider variety of mobilization exercises. This is better for body awareness and distributes stimulation more evenly throughout your body and your day.
Microbreaking

Probably no group of people can benefit more from regular, small batches of mobilizations than chair-bound office workers, followed closely by cashiers and others who are more or less stuck in one position and/or activity while working.
For all of you, “microbreaking” — taking small, regular, stimulating breaks — is the most important new concept in ergonomics. Stop worrying as much about how your workstation is arranged, and start thinking about how you use it!
Mobilizing is an ideal way to spend your microbreaks. Three or four times an hour, even if it’s only for thirty seconds or a minute, you should not just be getting up and changing your position, but dousing your nervous system and cranky muscles with movement.
See Microbreaking: Lots of little breaks may help compensate for too much time spent in chairs.
Conclusion: one more time, why and how in just a few words
Let’s wrap up by condensing this whole article into one brief explanation:
The most efficient exercise method for helping muscles and joints heal is to “massage them with movement,” providing just enough stimulation to facilitate healing, but not so much to aggravate. Mobilizing as soon as possible is proven to reduce recovery time from injury and surgery, and these benefits probably extend into recovering from chronic pain problems as well, especially those that involve muscle knots (which is most of them).
To do it, simply move rhythmically, shortening and lengthening muscles — basically, stretch one way and then the other, neither fast nor slow, pushing hard enough to be interesting but not hard enough to make anything worse. This is very much like squirming when stiff, only more repetitive and optimistic. The following numbers are roughly appropriate for most rehabilitation:
- 1–5 relevant mobilization exercises per workout
- 20–50 repetitions per side, or per direction for each exercise
- 1–3 workouts per day
- 3–7 days
For maintenance and prevention, smaller and more frequent batches of mobilizations are ideal.
Oh, and one more thing …
Did you find this article useful? Interesting? Maybe notice how there’s not much content like this on the Internet? That’s because it’s crazy hard to make it pay. Please support (very) independent science journalism with a donation. See the donation page for more information & options.
About Paul Ingraham

I am a science writer in Vancouver, Canada. I was a Registered Massage Therapist for a decade and the assistant editor of ScienceBasedMedicine.org for several years. I’ve had many injuries as a runner and ultimate player, and I’ve been a chronic pain patient myself since 2015. Full bio. See you on Facebook or Twitter., or subscribe:
Appendix A: The Chinese influence
I have been practicing t’ai chi and qigong since I was fifteen years old, when I first took lessons from an unlikely teacher, Prince George’s Sam Masich. Not much older than I was at the time, just twenty or so, Sam had recently returned from China, where he had won an international competition. Prince George, despite being a bit of a red-necked, backwater place, has a surprising way of producing talented people!
I am grateful to Sam for getting me off on the right foot with t’ai chi. I learned early that t’ai chi was practical as well as artful. Sam loved the martial aspects of t’ai chi, and would gleefully demonstrate how various poses related to the fighting stances of kung fu. To this day, I still notice how practically every t’ai chi student — they can often be seen on downtown Vancouver’s waterfront — still overextend themselves, reaching and leaning much too far, not realizing that t’ai chi is all about balance and grounding.
T’ai chi is also all about movement. The Chinese really get the idea of “use it or lose it.” In fact, t’ai chi is just one ingredient in a vast stew of ideas called “qigong,” which is basically “Chinese calisthenics.” Mobilization is qigong: gentle, rhythmic exercise.
Qigong, less well-known in the West, is extremely popular in China. The Chinese do it because it is a really smart form of exercise: stimulating enough to be useful, gentle enough to be useful into old age.25 While I was still in school, I recognized the similarity between qigong and the “early mobilization” of acute injury rehabilitation. Yet the Chinese don’t just use qiqong for recovery from recent injuries: they also use it as preventative medicine, to treat chronic health problems (which traditional Chinese medicine is so generally adept at treating), and as a lifelong constitutional26 with the intention of extending longevity.27
I started prescribing qigong exercises as soon as I was in practice, in 2000, but I didn’t call them qigong exercises. I just took the Eastern mysticism out of it — there is plenty of “woo woo” in qigong! — and started selecting exercise that specifically stimulated the joints and soft tissues I felt were most relevant to the pain problems and injuries my clients were bringing to me.
Appendix B: Case study of mobilizing a “neck crick”
Let’s look at the case of a neck crick in a little more detail. Why mobilize a neck crick? Neck cricks are caused by a combination of joint and muscular dysfunction, and usually respond well to stimulation. Neck range is limited by definition, and almost invariably increases with repeated gentle neck circles.
For a fresh, 2-day old severe neck crick, I would prescribe multiple large sets of neck circles each day, probably 3 sets of 80 (40 in each direction), with a good prognosis: based on my clinical experience, most people should be feeling much better after the first day of mobilizing, and will be almost completely recovered by the third day of mobilizing.
Is that actually any better than normal recovery time? It’s true, neck cricks generally do resolve on their own. However, it’s extremely common for them to bother people for three weeks, so getting that down to three days is a pretty good deal.
The neck circle is one of the simplest of all mobilizations: rolling the head around is pretty easy! I caution patients about the back of the circle, because the neck can feel uncomfortably crunchy in extension. But if it’s not distressing, it’s not a concern.
The trick is just to get the right intensity. If you only have 20˚ of right side bending … then that’s all you do. With every circle, you just nudge the edge of that range. Somewhere between thirty and forty turns, that range will probably increase to 25˚, if not on the first set, then on the second; if not on the first day, then on the second.
Appendix C: Mobilization Exercises Reference Chart
The following chart summarizes several mobilization exercises and what they are best used for — other than mild pain and stiffness in the area, which is a given. Click the green links to jump to more detailed descriptions below. I’m sorry there aren't videos or even photos. It’s on the to-do list!
| Mobilization | Summary | This mobilization is especially good for … |
|---|---|---|
| Abdominal Lift | Blow your breath out, and then suck your gut in strongly while holding your breath. | |
| Cats and Dogs | Straight from yoga: flex and extend your back while on your hands and knees. | |
| Chest Opening and Closing Mobilization | Spread your arms wide — a classic “good morning” stretch — and then collapse and give yourself a hug. | |
| Chest Rotations | Roll your chest in a slow-motion hoola hoop movement. This one is difficult for the coordination-challenged, but rewarding. | |
| Deep Gluteal Mobilization | Sit, cross one leg over the other, and lean forward. Then spread the feet and push the knees in and down. Far superior to a common physiotherapy stretch prescribed for sciatica and piriformis syndrome. | |
| Doorway Pectoralis Major Mobilization | Alternately stretch and contract the pectorals with the help of a doorframe. | |
| Foot Circles | Just roll the feet in circles. Simple, surprisingly difficult, and helpful for a wide variety of lower leg and foot problems. | |
| Forearm Mobilizations, seated | Sit on the edge of a bed and alternately bend your wrists forward and back on the mattress, with locked elbows. A deliciously stimulating sensation for computer users and cashiers. | |
| Forearm Mobilizations, standing | Bend your wrist back and forth with a locked elbow. Not as satisfying as the seated version (see Forearm Mobilizations, seated) but often more convenient. | |
| Iliopsoas Mobilization | Alternate between flexing and externally rotating the hip (contraction), and then doing an ordinary lunge with the back foot turned in (stretch). Great for chair-bound office workers especially. | |
| Iliotibial Band Mobilization | This is a complex “walking” stretch derived from taijiquan, which I think is much more effective than conventional iliotibial band stretches (for whatever ITB stretching is worth). | |
| Neck Circles | Roll your head in a circle. Incredibly useful for a huge array of common upper back, shoulder, neck and headache problems. | |
| Neck Flexor Mobilizations | Alternate between pulling the chin towards one side of the chest, and then tilting the head backward and to the opposite side. Sort of … | |
| Pelvic Circles | Swing the hips in a circle. This is a simple but powerful mobilization for low back pain and sciatica. | |
| Rotator Cuff Mobilizations | Rotate the humerus back and forth in the shoulder joint with a complex alternating motion. A complex but important mobilization. | |
| Spinal Twist Mobilization | While standing, turn your upper body back and forth, twisting the spine. | |
| Standing Forward Bend | Straight from yoga: touch your toes and then stand up with a rolling motion of the spine. | |
| Stick-Yer-Bum-Out | Stick your bum backwards and out to one side while twisting the spine. This reaches deep into one side of the low back. Then reverse the motion, and do the other side. | |
| Supine Lumbar Twists | Lying down, roll your pelvis and shoulders in opposite directions, back and forth. Supine lumbar twists are really pleasant, almost luxurious. | |
| Wide Arm Circles | Swing the arms in wide circles. One of the simplest of all mobilizations, and very helpful for many shoulder problems. | |
| Wrist Circles | Roll your wrists around in circles. Just like ankle rolls, this is surprisingly tiring! |
Abdominal Lift
Summary: Blow your breath out, and then suck your gut in strongly while holding your breath.
This is a classic yogic exercise, best known as a longevity exercise for its stimulating effect on the internal organs. It is also a powerful abdominal strengthener, and is vital for mastering many breathing techniques. Stand with your upper body supported on your knees. Take at least three deep breaths to prepare yourself for each lift. When you feel you have oxygenated sufficiently, blow all of your air out, hold your breath, and then suck your belly in hard against your spine. Particularly focus on your low belly, below the navel. Hold the position and your breath for several seconds (go as long as you can). Relax the belly before breathing again (if you try to breath first and then relax, it can hurt a bit). Repeat at least three times, or until you are exhausted. The best use of this exercise is three lifts per morning for the rest of your life.
This exercise is good for:
- stress
- constipation
- mild digestive disturbance
- practicing good diaphragmatic breathing
Cats and Dogs
Summary: Straight from yoga: flex and extend your back while on your hands and knees.
This one is straight from yoga. Stand on your hands and knees. Alternately arch and bow your back, starting the movement in the pelvis and letting it ripple up your spine to your head. Avoid moving the head prematurely.
This exercise is good for:
Chest Opening and Closing Mobilization
Summary: Spread your arms wide — a classic “good morning” stretch — and then collapse and give yourself a hug.
This exercise duplicates a familiar natural stretch that most of us do automatically in the morning or after getting up from a lot of sitting: spread your arms way back and lift your chest up. Now, to turn it into a mobilization, simply reverse the movement: reach your arms strongly across your chest and go “hunchbacked.”
This exercise is good for:
- low back pain
- upper back pain
- chest tightness
Chest Rotations
Summary: Roll your chest in a slow-motion hoola hoop movement. This one is difficult for the coordination-challenged, but rewarding.
This exercise looks something like a dance move. It is a challenging mobilization exercise for the thoracic cage. Begin by lifting your sternum upwards and outwards. Then push your ribs outwards towards each point on the compass in a smooth circle: up and fowards, up and left, up and back, up and right, and up and forward once more. Your shoulders must be relaxed! This is not a shoulder exercise! Also, your head and pelvis must be still, isolating the movement to the thoracic region. Good luck! This takes time and practice to master.
This exercise is good for:
- low back pain
- upper back pain
- tight chest
Deep Gluteal Mobilization
Summary: Sit, cross one leg over the other, and lean forward. Then spread the feet and push the knees in and down. Far superior to a common physiotherapy stretch prescribed for sciatica and piriformis syndrome.
Starting from a seated position, place your ankle on the stretch side over your knee on the other side. Let your lifted knee relax downwards for a moment, and then begin to lean forward from your pelvis. Avoid simply slumping forward, which is useless. Visualize pushing your belly button between your legs. Now do this on the other side, to even yourself out, even if you have symptoms only on one side. Now, to complete the mobilization for both sides, place your feet widely on the floor, and drop your knees straight down towards the floor.
This exercise is good for:
- low back pain
- sciatica iliotibial band syndrome
- piriformis syndrome

Doorway Pectoralis Major Mobilization
Summary: Alternately stretch and contract the pectorals with the help of a doorframe.
Stand in a doorway and reach out to one side. With your elbow trapped against the doorframe, step forward slightly with the leg on the stretch side, and push your shoulder on the stretch side forward and down. Hold for a few seconds, and then contract the muscle by stepping away and pressing your hands strongly together.
This exercise is good for:
- chest tightness
Foot Circles
Summary: Just roll the feet in circles. Simple, surprisingly difficult, and helpful for a wide variety of lower leg and foot problems.
Rotate each foot in a circle, first one direction and then the other. The movement must be slow, controlled and complete. You will be amazed at how tiring this is! Partly this is because of the common trigger points in the calf and shin muscles, and partly it’s because our ankle coordination is usually quite poor. You might notice, for instance, that you have quite a bit of trouble smoothly rolling one direction or the other. The action becomes tiring in the same way that trying to wiggle your ears is “tiring.”
This exercise is good for:
Forearm Mobilizations, seated
Summary: Sit on the edge of a bed and alternately bend your wrists forward and back on the mattress, with locked elbows. A deliciously stimulating sensation for computer users and cashiers.
Sit on the edge of your bed or any other firm surface where there is space to put your hands down on either side of you. Stretch the hand back by placing the palm face down with your fingers towards you. Lean into it a bit and then release. Repeat this on the other side. Now go back to the first hand again and do the opposite: place the back of your hand downwards, fingers still pointing towards you. Lean into it for a moment, and then switch to the other side. Now just rhymically move back and forth: right, left, right, left, and so on. Keeping your elbows locked helps.
This exercise is good for:
- tennis elbow
- typists
Forearm Mobilizations, standing
Summary: Bend your wrist back and forth with a locked elbow. Not as satisfying as the seated version (see Forearm Mobilizations, seated ) but often more convenient.
This mobilization alternately stretches each side of your forearms, and is derived directly from the forearm and wrist stretches practiced in the Japanese martial art of Aikido. Do one arm at a time. The first stretch is easy: simply lock the elbow, turn the inside of the forearm face up (supinated), and then pull the fingers back to strongly extend the wrist. Stretching the back of the forearm is trickier: stick your arm straight out, and turn the palm face down and continue rotating it until it is facing out. Now, lay your other hand over top, grab it, and twist it even further. Add a little extra pressure to push the wrist into flexion. The final position is nearly impossible to describe, so the diagram of this exercise is especially useful! There are a couple of other interesting things to note about this mobilization: first of all, by my own rules, it’s not really a mobilization, because there is little or no muscle contraction involved, just passively stretching one way and then the other. A true mobilization is Wrist Circles , which actually uses the forearm muscles. However, the stretching sensations in this exercise are so typically pleasant that I recommend it anyway. Also, note that in the wrist-flexed position, you can get a very strong and pleasurable stretch by pushing the back of the wrist up against a wall — try it!
This exercise is good for:
- tennis elbow
- typists
Iliopsoas Mobilization
Summary: Alternate between flexing and externally rotating the hip (contraction), and then doing an ordinary lunge with the back foot turned in (stretch). Great for chair-bound office workers especially.
This mobilization stimulates some obscure but important hip flexors that are held in a shortened position while sitting. Step forward with your right foot in a mild “lunge” position, like a fencer. This opens and stretches the LEFT hip and iliopsoas muscle. Turn the back (left) foot sharply inwards (pigeon-toed) — this increases the elongation of iliopsoas a little more. Your iliopsoas is now quite long, but to push it one more notch, simply shift your hips down and forward a little more. Hold for a moment, and then stand up. Now contract the iliopsoas: lift the inside of the left foot as high as you can, as though you are trying to lift a glass of water on the inside of your foot. That completes the cycle for the left side. Repeat several times to mobilize the iliopsoas on the left side. Then switch to the other side and repeat several more times.
This exercise is good for:
Iliotibial Band Mobilization
Summary: This is a complex “walking” stretch derived from taijiquan , which I think is much more effective than conventional iliotibial band stretches (for whatever ITB stretching is worth).
The iliotibial band mobilization is a dynamic stretch that occurs as you are moving, teaching the muscles that control the tension on the ITB to be responsive, shortening and lengthening as needed. By “freezing” the movement in the right place, you can also stretch the ITB more powerfully than by any other method I know of.
Begin by standing. Step forward the distance of a normal stride, placing your front foot in line with your back foot or even slightly across the midline. The toe of the forward foot should be pointed outwards. The forward leg is not the leg you’re stretching—the back leg gets the stretch.
Crouch deeply, lowering the knee of the back leg almost to the ground. As you do so, push your hip (of the back leg) out to the same side, and your knee (of the back leg) to the far side. Then stand up, step forward with your other leg, and repeat on the other side.
Another important element of this mobilization is arm movement (not shown in diagram). It may take some practice to integrate this step, especially while moving. However, the stretch is strengthened significantly by reaching up and away from the stretch side. That is, when dropping the right knee and stretching the right ITB, reach upwards, backwards and to the left, leaning away from the front right corner of the pelvis.
Here’s a video of the stretch being doing mobilization-style (continuously moving in and out of the stretch, rather than holding it).
This exercise is good for:
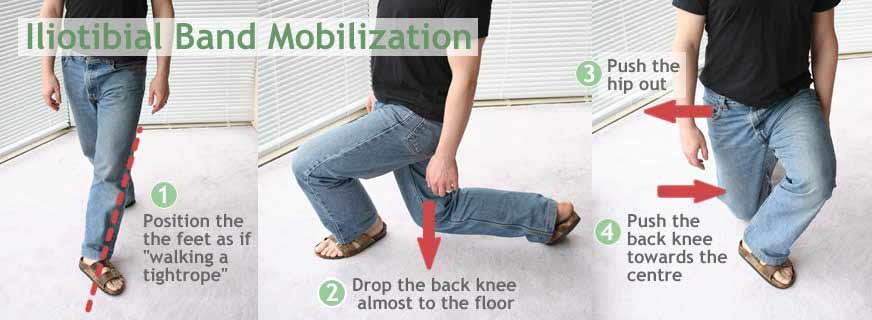
That picture gives you a basic idea, but it’s not enough, so here's a little demonstration video of this tricky exercise!
Neck Circles
Summary: Roll your head in a circle. Incredibly useful for a huge array of common upper back, shoulder, neck and headache problems.
Roll your head in a circle, using your pain free range of motion. That is, roll as far as you can in every direction, as long as it doesn’t hurt. You want to right up to “edge” of any discomfort, and perhaps just slightly further ... but keep it easy. Note: when your head is rolled backwards, your neck may feel crunchy. You can skip that part of the circle if it bothers you, but it’s harmless unless obviously uncomfortable.
This exercise is good for:
Neck Flexor Mobilizations
Summary: Alternate between pulling the chin towards one side of the chest, and then tilting the head backward and to the opposite side. Sort of …
This is a difficult exercise to visualize. Basically, for the left side (for example), lift your chin up and away to the left, while pulling the left shoulder down and back. This opens up the left side of the throat and chest. Another way of thinking about it: try to get your left ear as far above and behind the sternum as possible. In more detail: (1) lean the head to the RIGHT, pulling the right ear towards the right shoulder, (2) tilt the head BACK, (3) turn the head the LEFT, (4) pull the left shoulder down and back. To complete the exercise and make it a full mobilization, you also need to atlernate stretch with contraction of these muscles: simply try to touch your cheek and your left shoulder.
This exercise is good for:
Pelvic Circles
Summary: Swing the hips in a circle. This is a simple but powerful mobilization for low back pain and sciatica.
Stand and begin to swing your hips in a broad circle. Gradually expand the circle until you are pushing your pelvis as far as possible towards each point of the compass. If you have back pain, one part of the circle is likely to be extremely stiff or painful, so just keep it easy, do only as wide a circle as feels comfortable, even if that’s very small.
This exercise is good for:
Rotator Cuff Mobilizations
Summary: Rotate the humerus back and forth in the shoulder joint with a complex alternating motion. A complex but important mobilization.
This exercises is a little tricky, but quite valuable. Its purpose is to stimulate the rotator cuff musculature, which is infamous for always getting injured (you’ve probably heard of “rotator cuff injuries”). Stimulating the rotator cuff is often important, because trigger points in the rotator cuff musculature often have widespread effects in the shoulder, arm and even the wrist. This is how you do it: the mobilization alternates between two quite different movements, one which twists the upper arm inwards, the other outwards. To do the first one, place your fists on your hips (with your wrists bent backwards), and pull your elbows together. Hold that stretch briefly. Now, to do the second movement, tuck your elbows right in to your side, spread the hands outwards, and then try to push the elbows forward and together. Alternate back and forth between both movements.
This exercise is good for:
- frozen shoulder
- arm pain
Spinal Twist Mobilization
Summary: While standing, turn your upper body back and forth, twisting the spine.
While standing, turn your body as far to the left or right as possible, twisting your spine thoroughly. Your pelvis should remain more or less aimed forward. Now go the other way. You can do this mobilization quite quickly, so especially large numbers of repetitions are often appropriate when trying to solve a problem. You may also find that you enjoy almost throwing yourself back and forth, letting the limits of spinal rotation stop you: this is okay if it feels good to you, but do use some caution with this style of course.
This exercise is good for:
Standing Forward Bend
Summary: Straight from yoga: touch your toes and then stand up with a rolling motion of the spine.
Stand with your feet shoulder width apart and toes pointed slightly inwards, knees unlocked — this is not a hamstring stretch. Breathe steadily for the duration of the exercise. Begin by lowering your chin to your chest and continue to flex your intervertebral joints one at a time. The lower parts of the spine should remain erect for as long as possible. Continue until your entire upper body is hanging from your hips, and make sure your head is a relaxed dead-weight at the end of the spine. At this point, you have two choices for getting back upright: for the first 3-5 repetitions, you should (a) squat down, slowly straighten your back, and then stand up using the strength of your legs; but once you are warmed up a bit, you can (b) simply reverse the spinal movement instead, rolling up instead of down, lifting the vertebrae back into place one by one, starting with the low back and moving upwards.
This exercise is good for:
Stick-Yer-Bum-Out
Summary: Stick your bum backwards and out to one side while twisting the spine. This reaches deep into one side of the low back. Then reverse the motion, and do the other side.
This unusual mobilization reaches the low back and gluteus maximus in a way that no other exercise can, stimulating that hard-to-reach spot in the very bottom “corner” of the low back, just above the dimple. Stick your bum out as though you are going to sit down on a stool that is well behind you and off to one side. Your knees must bend. Round your low back like the top of a ball, lean your torso in the other direction (i.e. bum goes left, torso goes right), and twist your shoulders to face back towards the middle. (The further you lean and twist, the further the stretch will “reach” into your upper back.) To conclude, stand up and lean back a bit, clenching your gluteal and low back muscles firmly. Now alternate from side to side: left, clench, right, clench, left, clench, etc.
This exercise is good for:

Supine Lumbar Twists
Summary: Lying down, roll your pelvis and shoulders in opposite directions, back and forth. Supine lumbar twists are really pleasant, almost luxurious.
This is a especially satisfying mobilization found in various forms in many different exercise traditions, especially yoga. Lie down face up. Roll your pelvis and legs to one side, using the weight off the top leg to twist your lower body one way, while your upper body remains relatively fixed on the ground. Experiment with positioning. You will mainly notice a deep torquing of the spine and deep stretches in the hips. Go back and forth slowly but steadily.
This exercise is good for:
Wide Arm Circles
Summary: Swing the arms in wide circles. One of the simplest of all mobilizations, and very helpful for many shoulder problems.
Standing, swing both arms in circles as wide as you can manage. Divide your set into several circles in one direction, and the several in the other direction. Typically, this exercise is done specifically when there is pain or limited range in the shoulder, and it is easy to overdo it. Tinker with the size of the circle so that you can actually comfortably do as many repetitions as desired. For instance, you may easily be able to do 10 circles in one direction, but really start to feel tired by 20 ... so don’t lift your arms as high!
This exercise is good for:
- headaches
- rotator cuff injuries
Wrist Circles
Summary: Roll your wrists around in circles. Just like ankle rolls, this is surprisingly tiring!
This is an extremely simple mobilization exercises. Roll the wrist in circles, first one way and then the other. You will probably be surprised by how quickly this tires your arms out: the forearm muscles are not usually accustomed to repeated contraction, even gentle contraction. Make the circles small enough that you can repeat them as many times as you need to.
This exercise is good for:
- carpal tunnel syndrome
- tennis elbow
Related Reading
- How to Do Joint Mobility Drills, by Todd Hargrove: some excellent primer material quite similar in spirit to this article, but with some great discussion of why mobilizations are a good idea.
- Endurance Training for Pain & Rehab — Why endurance training might be a wise alternative to strength training (especially when healing from an injury)
- Microbreaking — Lots of little breaks may help compensate for too much time spent in chairs
- PF-ROM Exercises — ‘Pain-free range of motion’ or early mobilization exercises can help you heal
- Quite a Stretch — Stretching science has shown that this extremely popular form of exercise has almost no measurable benefits
- The Trouble with Chairs — The science of being sedentary and how much it does (or doesn’t) affect your health and back pain
What’s new in this article?
2023 — Complete descriptions of all mobilization exercises are now integrated into this page. The table of contents also got an upgrade.
2018 — Science update, cited Kim on the effect of early mobilization on recovery from surgical repair of shoulder trauma.
2004 — Publication.
Notes
- Ingraham. Quite a Stretch: Stretching science has shown that this extremely popular form of exercise has almost no measurable benefits. PainScience.com. 35519 words.
- Use it or lose it. Motion is lotion. Fake it until you make it. Flex it to protect it. Squirmin’ is learnin’. Groove to improve. Mobilize or fossilize. If you want to improve it, move it.
- For instance, consider shoulder trauma: most people, even most surgeons, probably still believe that a ripped-up shoulder probably needs to be braced after surgical repair. Au contraire! Kim et al. compared early mobilization to immobilization for such patients, and found … no difference. A big fat nothing-burger. Mobilization didn’t help, but it’s important that it didn’t hurt either — moving was not a problem even for seriously injured shoulders.
- Consider a modern example:
I had a massage therapy client in the 2000s who broke her arm and was told by her doctor: “Look, I can put this in a cast and it will be nice and safe, or we can leave it out and it will heal three weeks faster if you can protect it properly until then.” She chose to skip the cast, and was simply very careful with her arm for a little while. Sure enough, the wound was healed in excellent time. Even though she was very careful with it, the gentle stresses of gravity and slight movements alone were enough to stimulate accelerated healing.
- Oldmeadow LB, Edwards ER, Kimmel LA, et al. No rest for the wounded: early ambulation after hip surgery accelerates recovery. ANZ J Surg. 2006 Jul;76(7):607–611. PubMed 16813627 ❐
From the abstract: “Early mobilization after hip fracture surgery accelerates functional recovery and is associated with more discharges directly home and less to high-level care.”
- Hagen KB, Jamtvedt G, Hilde G, Winnem MF. The updated cochrane review of bed rest for low back pain and sciatica. Spine. 2005 Mar;30(5):542–546. PubMed 15738787 ❐
From the abstract: “For people with acute low back pain, advice to rest in bed is less effective than advice to stay active.” There is even “high quality evidence” that bed rest leads to more pain.
- Vroomen PC, de MC Krom, Wilmink JT, Kester AD, Knottnerus JA. Lack of effectiveness of bed rest for sciatica. N Engl J Med. 1999 Feb 11;340(6):418–23. PubMed 9971865 ❐ PainSci Bibliography 56953 ❐
In this sciatica study, researchers assigned 183 subjects “either bed rest or watchful waiting” for two weeks and found that “bed rest is not a more effective therapy than watchful waiting.” Nor is it less effective. The results were exactly the same. If that sounds like no big deal, consider the difference in the lives of those patients: two weeks of bed rest, compared to two weeks of going about your business!
- Sorrenti SJ. Achilles tendon rupture: effect of early mobilization in rehabilitation after surgical repair. Foot Ankle Int. 2006 Jun;27(6):407–410. PubMed 16764795 ❐
From the abstract: “Surgery combined with early mobilization reduces range of motion loss, increases blood supply, and reduces the degree of muscle atrophy that typically occurs after Achilles tendon rupture, thereby decreasing the time to resumption of normal activities.”
- See Mealy, Vassiliou, McKinney, and Schnabel.
- Lamb SE, Marsh JL, Hutton JL, Nakash R, Cooke MW. Mechanical supports for acute, severe ankle sprain: a pragmatic, multicentre, randomised controlled trial. Lancet. 2009 Feb 14;373(9663):575–581. PubMed 19217992 ❐
It’s been in vogue in physical therapy for a long time now to “mobilize” injuries as quickly as possible — probably too much in vogue. In the zeal to get people on their feet again ASAP, serious sprains — which are worse than fractures in some ways — are almost never put in a cast. Turns out that’s a mistake. A 2009 experiment published in the Lancet presents clear evidence that a full cast for a severe ankle sprain is superior to the almost universal practice of using braces and tubular compression bandages. The editors write, “This elegant study highlights the need for trials to address common problems.”
- Soligard T, Myklebust G, Steffen K, et al. Comprehensive warm-up programme to prevent injuries in young female footballers: cluster randomised controlled trial. BMJ. 2008;337:a2469. PubMed 19066253 ❐ PainSci Bibliography 56160 ❐
- There were also undoubtedly many differences, and the research I’m citing is certainly not perfectly applicable to mobilizations. However, it’s definitely somewhat applicable — nearly any moving warm-up counts as some kind of mobilization.
- Soligard T, Nilstad A, Steffen K, et al. Compliance with a comprehensive warm-up programme to prevent injuries in youth football. Br J Sports Med. 2010 Sep;44(11):787–93. PubMed 20551159 ❐ PainSci Bibliography 54998 ❐
- “Mobilizations” as I have described them here are a more general, accessible concept than neurodynamic mobilization, but both techniques share rationales and assumptions. I assume that whatever benefits are provided by neurodynamic mobilizations are probably somewhat encompassed by the technique I recommend. If you do mobilizations, you are going to be doing some neurodynamic mobilizations as well — sloppily and essentially by accident, but perhaps better than nothing. Neural mobilization one way to understand why mobilizations are helpful. See Neurodynamic Stretching: Stretching and stimulating nerves to treat neuropathy… hopefully.
- For instance: Puetz TW, O'connor PJ, Dishman RK. Effects of chronic exercise on feelings of energy and fatigue: a quantitative synthesis. Psychol Bull. 2006 Nov;132(6):866–876. PubMed 17073524 ❐
This is study of other studies (meta-analysis) that concluded that exercising regularly reduces feelings of fatigue. Intriguingly, it also identified some clues that the effect might be induced by placebo.
And of course there are countless other kinds of research showing an incredible variety of exercise benefits. - Or consider the enormous body of cultural and medical wisdom that constitutes the foundation of t’ai chi and qigong in China. See Appendix A for more.
- Hopefully it’s perfectly obvious the healing tissues are threatened by overexertion! More important, and less obvious, is that tissues harbouring myofascial trigger points are at risk. Trigger points are easily sustained and aggravated by overexertion. Given their clinical importance — their tendency to cause, complicate or even replace virtually any other musculoskeletal problem — the risk of irritating them with therapeutic exercise is not trivial. See Mense.
- See Strength Training for Pain & Injury Rehab and Quite a Stretch.
- The Trouble with Chairs
- This is actually really important in rehabilitation: a lot of clever rehabilitation and therapeutic exercise concepts look great on paper, but fail miserably when you ask real people to do them. The actual ease of usage of mobilizations is one of their strongest benefits.
- It’s a morbid example, but consider the effectiveness of immobilization as a torture method. Victims suffer terrible agony and degeneration surprisingly swiftly. Strange as it may seem to bring this up, consider the physiological implications: why does being still hurt so much? Physiologically? I assume it’s because we are hard-wired in many different ways to avoid stagnancy, because it’s actually dangerous. Even trying to sit still for meditation soon causes pain.
- I remember having a debate with a colleague about the difference between stretching and mobilizing, only to discover that there was no difference between his kind of stretching and my mobilizing. He simply thought of mobilizations as the “correct way to stretch” — as a kind of stretch. Which, of course, they are. However, I consider mobilizing to be sufficiently different from stretching to deserve its own classification.
- The case for this is thoroughly explored in Quite a Stretch. Considerable scientific evidence is presented. It’s a difficult article to read without wondering why anyone ever bothered stretching in the first place.
- This possibility is considered in the article Quite a Stretch.
- See note 9.
- Cohen K. The way of qigong: the art and science of chinese energy healing. Ballantine; 1997.
- There are numerous studies suggesting general systemic benefits to meditation and meditative exercise like t’ai chi, qigong and yoga. It’s not all that important to my point, so I won’t review them here.

